

Google. Neurology vs Psychiatry. Neurology and psychiatry are related fields - if for no other reason, because neurological disorders can often manifest as, and get misdiagnosed as, psychiatric ones.

But what's the borderline between neurology and psychiatry? What makes one disease "neurological" and another "mental"? Are some psychiatric disorders more "neurological" than others? It's a rather philosophical question and you could discuss it for as long as you wanted. Rather than doing that I thought I'd have a look to see which disorders are, at the moment, considered to fall into each category. To do this I did a quick search the archives of two journals, Neurology which the world's leading journal of... well, guess, and the American Journal of Psychiatry. Some interesting results.
Guitarist refused to let the music die - SignOnSanDiego.com. Billy McLaughlin concert When: Thursday, 7 p.m.
Where: Neurosciences Institute, 10640 John Jay Hopkins Drive Cost: $25 general admission, $45 VIP. Most ALS May Stem from Protein Misfolding - in Neurology, General Neurology from MedPage Today. Amyotrophic lateral sclerosis (ALS) may be a disease of protein misfolding, according to a study that affirms that abnormal protein structure found in inherited cases plays a role in sporadic cases as well.
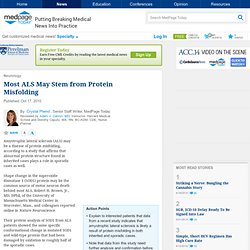
Shape change in the superoxide dismutase 1 (SOD1) protein may be the common source of motor neuron death behind most ALS, Robert H. Brown, Jr., MD, DPhil, of the University of Massachusetts Medical Center in Worcester, Mass., and colleagues reported online in Nature Neuroscience. Their protein analysis of SOD1 from ALS patients showed the same specific conformational change in mutated SOD1 and wild-type protein that had been damaged by oxidation in roughly half of the sporadic cases. "These results indicate that at least a subset of sporadic ALS cases contain wild-type SOD1 proteins that are structurally similar to familial ALS-linked SOD1 mutant proteins," Brown's group wrote in the paper. None of the 17 control cases without ALS stained positive. false.
McLeod syndrome. Clinical features[edit] Laboratory features[edit] McLeod syndrome is one of only a few disorders in which acanthocytes may be found on the peripheral blood smear.
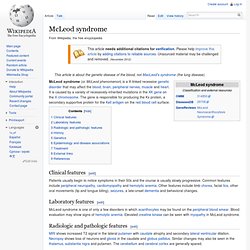
Blood evaluation may show signs of hemolytic anemia. Elevated creatine kinase can be seen with myopathy in McLeod syndrome. Radiologic and pathologic features[edit] MRI shows increased T2 signal in the lateral putamen with caudate atrophy and secondary lateral ventricular dilation. History[edit] McLeod syndrome was discovered in 1961 and, as with the Kell antigen system, was named after the first patient in which it was found: a Harvard dental student Hugh McLeod, whose red blood cells were observed to have weak expression of Kell system antigens during blood donation,[1] and his red cells were found to be acanthocytic (spiky) under the microscope.
Genetics[edit] The phenotype may be present without the syndrome presenting.[5] Epidemiology and disease associations[edit] Treatment[edit] External links[edit] Neuroscience. Activities - Deep Brain Stimulation Surgery. Treating Tourette Syndrome with Deep Brain Surgery. It is easy to be convinced that deep brain stimulation (DBS) works to improve Tourette syndrome.
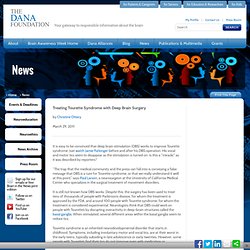
Just watch Jamie Furlonger before and after his DBS operation. His vocal and motor tics seem to disappear as the stimulation is turned on. Is this a "miracle," as it was described by reporters? “The trap that the medical community and the press can fall into is conveying a false message that DBS is a cure for Tourette syndrome, or that we really understand it well at this point,” says Paul Larson, a neurosurgeon at the University of California Medical Center who specializes in the surgical treatment of movement disorders.
It is still not known how DBS works. Nervous system diagnostic terms flashcards. A Stroke Of Good Fortune Cures OCD? A 45 year old female teacher had a history of severe obsessive-compulsive disorder, along with other problems including ADHD.

Her daughter, and many other people in her family, had suffered the same problems and in a few cases had Tourette's Syndrome. But all that changed - when she suffered a stroke. This is according to a brief case report from Drs. Featured Neurologist: Charles Putnam Symonds. Charles Putnam Symonds was born in London, England to Charter Symonds, a surgeon at Guy’s Hospital and the Association of British Neurologists’ tenth President.
Symonds was educated at Oxford University's New College and Guy’s Hospital, where he trained under Arthur Hurst and Adolph Meyer. Symonds received his medical qualification in 1915. In 1919, he was appointed to National Hospital, Queen Square. The same year, he became the medical registrar at Guy's Hospital and was quickly promoted to neurologist. The relevance of Nash equilibrium to psychiatric d... [Theor Med Bioeth. 2011] - PubMed result. The Brain Observatory. MiR-16 Targets the Serotonin Transporter: A New Facet for Adaptive Responses to Antidepressants.
OLD Jeggsey. Why Night Owls Are More Intelligent than Morning Larks. Some people are night owls, and others are morning larks. What makes the difference may be their levels of general intelligence . Virtually all species in nature , from single-cell organisms to mammals, including humans, exhibit a daily cycle of activity called circadian rhythm . The circadian rhythm in mammals is regulated by two clusters of nerve cells called the suprachiasmatic nuclei (SCN) in the anterior hypothalamus.
Geneticists have by now identified a set of genes that regulate the SCN and thus the circadian rhythm among mammals. However, humans, unlike other mammalian species, have the unique ability, consciously and cognitively, to override their internal biological clock and its rhythmic outputs. While there are some individual differences in the circadian rhythm, where some individuals are more nocturnal than others, humans are basically a diurnal (day-living) species.
An analysis of a large representative sample of young Americans confirms this prediction.