

Untitled. She’s called Gemma.

She’s three years old. She fell into a canal,” said a senior nurse. “By the time her parents managed to get her out, apparently she’d already stopped breathing.” “Paramedics three minutes away,” called another nurse, holding the scarlet phone on which emergencies were called through. With a grace and efficiency akin to choreography, a team of professionals who moments beforehand had been as disparate as atoms, dispersed across the hospital, were poised around an empty resuscitation bed, waiting as one to swing into action. The consultant quietly confirmed each team member’s role. It was impossible to hear the paramedics’ handover above the screams of Gemma’s mother.
Too inexperienced to help, I hovered on the periphery, trying not to wear my shock visibly. On and on the crash team worked. Fifteen, 20 minutes must have passed. Not for one second did the team’s concentration dip. The smiles after she departed could not have been any broader. I worked fast. Untitled. Margaret Munro is a Vancouver-based journalist.
My father was preparing breakfast when his blood pressure dropped and he blacked out. Keeling over backward, he hit his head so hard it punched a hole in the wall. “Good thing I didn’t hit the stud,” he said in the emergency room at Nanaimo Regional General Hospital. Untitled. It was easy for my mother to call 911 and have him transported to the hospital.
But if he fell again, there would be no 911-like number for my mother to call for urgent assistance short of EMTs and ambulances. It would be easy for the emergency-room physician to admit my father again, and even put him in the intensive-care unit. But no one suggested that he and my mother get mental health care or see a grief counselor to cope with his new terminal diagnosis. The hospital was no place for my father to spend his last days. To thwart the medical system’s momentum to lard on ever more costly, unnecessary, and unwanted interventions—and to convince the medical staff we were serious about no—I took my father’s oxygen monitor off his finger, disconnected his cardiac monitor, insisted that the nurse remove his IV, and asked the physician to discharge him as soon as possible.
Judge dismisses suit against doctors accused of ignoring man’s wishes to stay alive. TORONTO — Two doctors were acting within the rules and providing adequate care to an elderly patient when they imposed a “do not resuscitate” order on the man without notifying him or his substitute decision maker, an Ontario judge ruled this week.
Ontario Superior Court Justice Peter Cavanagh defended the actions of Dr. Donald Livingston and Dr. Martin Chapman as he dismissed a $2.2 million lawsuit against the two physicians who treated Douglas DeGuerre. “Dr. Caring. Jamanetwork. Key Points Question Is care for older adults with multiple chronic conditions that is aligned with their health priorities associated with improved patient-reported outcomes and reduced unwanted care?
Findings This nonrandomized clinical trial of 366 adults 65 years or older with multiple chronic conditions found that, although there was no difference in perception of whether their care was goal-directed or coordinated, participants receiving patient priorities care vs usual care reported a greater reduction in treatment burden, and their health records reflected more medications stopped and fewer self-management tasks and diagnostic tests added. Meaning This study’s findings suggest that aligning care with patients’ priorities may improve outcomes for patients with multiple chronic conditions.
Assessment of Self-reported Prognostic Expectations of People Undergoing Dialysis: United States Renal Data System Study of Treatment Preferences (USTATE) Key Points Question What are the prognostic expectations of people undergoing dialysis, and how do these relate to their treatment goals and preferences?
Findings In this cross-sectional survey study of 996 patients receiving maintenance dialysis at nonprofit facilities in 2 US metropolitan areas, most of the respondents were either uncertain about prognosis or had a prognostic expectation of more than 10 years. In adjusted analyses, these groups were less likely than those with a prognostic expectation of fewer than 5 years to report having documented their treatment preferences and to value comfort over life extension, and more likely to want cardiopulmonary resuscitation and mechanical ventilation.
PREPARE. 'Dying is not as bad as you think' - BBC Ideas. To treat or not to treat: find out what really matters to the patient. “What do you want?”
“Whatever you say, doctor.” “It would be helpful for me to know about your goals in life.” “Goals?” 10. Admitting Elderly Patients to the Intensive Care Unit—Is it the Right Decision? One of the most important decisions that a physician makes is whether to admit a patient to the intensive care unit (ICU).
The modern ICU provides a capacity for advanced monitoring and life support that is typically unavailable elsewhere in the hospital and is lifesaving for patients with a wide array of acute deteriorations in health. However, ICU care is also one of the most expensive, intensive, and intrusive endeavors in health care. Although patients admitted to the ICU account for approximately one-quarter of hospitalized patients, they account for half of total hospital expenditures in the United States, with costs estimated at $110 to $260 billion per year or approximately 1% of the gross domestic product.1-3 Furthermore, ICU care can be unnecessary, harmful, or futile.
How accurate is the 'Surprise Question' at identifying patients at the end of life? A systematic review and meta-analysis. - PubMed - NCBI. How Surrogates Decide: A Secondary Data Analysis of Decision-Making Principles Used by the Surrogates of Hospitalized Older Adults. The Symptoms of Protracted Dying. Jamanetwork. Alice Hodkinson, David Spitzer, and Iona Heath: Overdiagnosis of end of life – The BMJ.
Doctors are much more likely to cause problems by underdiagnosing end of life than by overdiagnosing it Apparently, “tens of thousands of patients are being prematurely warned they could be about to die because of a defective diagnostic method used across the NHS” (The Telegraph).
This “stone age” (MailOnline) diagnostic method is the well known “surprise question,” which asks doctors, “Would you be surprised if this patient died within the next × months?” And the “alarming new study” these newspaper articles refer to is a paper that looked at the accuracy and utility of doctors asking themselves the question.
The Charlie Gard story reveals what we won't accept about medicine. The parents of critically ill baby Charlie Gard, Connie Yates and Chris Gard, pose for the media with a petition, outside Great Ormond Street Hospital, in central London, Britain July 9, 2017.
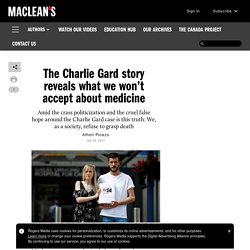
The parents want their son, who has a form of mitochondrial disease, to be able to travel to receive further treatment, after losing a long legal battle to give him experimental therapy in the United States. (Peter Nicholls/Reuters) It’s the most commonly cited phrase from the Hippocratic Oath, the binding document—one of the oldest in history—upon which physicians swear: “First, do no harm.” However, that four-word axiom doesn’t itself appear in the classical text of the pledge. Instead, there’s a promise to “apply dietetic measures for the benefit of the sick according to my ability and judgment; I will keep them from harm and injustice.” Born Aug. 4, 2016, Charlie has lived all but the first nine weeks of his life in London’s Great Ormond Street Hospital. The "surprise question" for predicting death in seriously ill patients: a systematic review and meta-analysis.
What makes a life worth living? The debate behind continuing life support - The Globe and Mail. Over the past 20 years, neuroscientist Dr. Adrian Owen has studied many patients who are minimally conscious or in a vegetative state. To assume they’re all unhappy is “extremely naive,” he says. End-of-life care: How to have a better death. IN 1662 a London haberdasher with an eye for numbers published the first quantitative account of death. John Graunt tallied causes such as “the King’s Evil”, a tubercular disease believed to be cured by the monarch’s touch. Others seem uncanny, even poetic. End-of-life care: A better way to care for the dying. A STROLL from Todoroki station, at the kink of a path lined with cherry trees, lies a small wooden temple. A baby Buddha sits on the sill. The residents of the Tokyo suburb ask the infant for pin pin korori.
It is a wish for two things. The first is a long, spry life. The second is a quick and painless death. Daily chart: What people want at the end of life. IN 2016 The Economist and the Kaiser Family Foundation, an American non-profit focused on health care, polled people in America, Brazil, Italy and Japan about their hopes and worries for their end-of-life wishes. We found that what is most important to people at the end depends on where they live. In America and Japan not burdening families with the costs of care was the highest-ranked priority. (The Japanese may be worrying about the cost of funerals, which can easily reach ¥3m, or $24,000; Americans may be worrying about medical bills, which can be ruinous.)
Serious illness conversations and capturing advance care planning. A doctor discovers an important question patients should be asked. This patient isn’t usually mine, but today I’m covering for my partner in our family-practice office, so he has been slipped into my schedule. Reading his chart, I have an ominous feeling that this visit won’t be simple. Treatment targeted at underlying disease vs palliative care in terminally ill patients: A systematic review. 'Modern Death': Doctor Pulls Back Curtain On The Slow Way We Die Now. Caiaimage/Sam Edwards/Getty Images Humans have had to face death and mortality since since the beginning of time, but our experience of the dying process has changed dramatically in recent history. Haider Warraich, a fellow in cardiology at Duke University Medical Center, tells Fresh Air's Terry Gross that death used to be sudden, unexpected and relatively swift — the result of a violent cause, or perhaps an infection.
Advances in Clinical Management: Cardiopulmonary Resuscitation for older people: the mirage of numbers. In June of the same year, the NEJM itself published a couple of letters to the director stressing that the data presented by American Heart Association researchers, whilst true, were also misleading. In another "icon-box", GeriPal summarized the same results but viewed from a global perspective, which could be explained as follows: out of 100 people aged 64 and over who received CPR during hospitalization, 49 did not survive the resuscitation attempts and 34 died during the subsequent stay. This means that 83 of the patients (49 + 34) showed as discharged dead and therefore only 17 were discharged alive.
Effect of the Goals of Care Intervention for Advanced Dementia. Do-not-resuscitate orders in cancer patients: a review of literature. The Decline of Tube Feeding for Dementia Patients. Photo from Parkinson’s disease was taking its toll on Joan Jewell. She could still respond to music, if a helper wheeled her to the Sunday concert at the Hebrew Rehabilitation Center in Boston, but she spent most of her time in bed. Sometimes she recognized family members; often she didn’t. The patient is Code 3 critical. Her frail, 90-year-old body is failing. How much should I do to save her life?' Functional Trajectories Among Older Persons Before and After Critical Illness. What doctors don’t learn about death and dying. The Dirty Secret About CPR in the Hospital (That Doctors Desperately Want You to Know) Mandate to obtain consent for withholding nonbeneficial cardiopulmonary resuscitation is misguided.
Saving Sid. An unforgettable call The first friend or family member to hear the news was Shouvik Datta . A Nursing Story – with ZdoggMD props (not a fangirl post, Dogg) Barriers to Goals of Care Discussions With Seriously Ill Hospitalized Patients and Their Families: A Multicenter Survey of Clinicians.
CPR survival statistics - metanalysis. This is not Casualty – in real life CPR is brutal and usually fails. When Do Not Resuscitate Is a Nonchoice Choice: A Teachable Moment. How we used to die; how we die now. Comparison of Site of Death, Health Care Utilization, and Hospital Expenditures for Patients Dying With Cancer in 7 Developed Countries. Hearing Others’ Perspectives When We Hear, “Do Everything!”
A Surgery Standard Under Fire. Force-Feeding: Cruel at Guantánamo, but O.K. for Our Parents. Third of dying hospital patients marked to receive CPR against their wishes, Canadian study says. 'The day I meet you in the emergency department will probably be one of the worst of your life' When 'Doing Everything' Is Way Too Much. Why is CPR being used for end-of-life care? Study: suffering at end of life is getting worse, not better. Personalizing Death in the Intensive Care Unit: The 3 Wishes Project: A Mixed-Methods Study.
When Do Not Resuscitate Is a Nonchoice Choice: A Teachable Moment. Why I Hope to Die at 75. Deferring death can mean a life of suffering. End-of-life chemotherapy: Does it do more harm than good? Wish program aims to make dying in a hospital ICU more humane. Can We Have a Fact-Based Conversation About End-of-Life Planning? B.C. hospital kept patient alive for 10 days because family’s culture did not accept brain death. Conservative (non dialytic) management of end-stage renal disease and withdrawal of dialysis. Conservative Management of End-Stage Renal Disease without Dialysis: A Systematic Review. It’s Not Just About ‘Quality of Life’ Teaching doctors when to stop treatment.