

House committee to add oversight controls to VA's EHR project. Lawmakers on Thursday told leaders from the Veterans Affairs Department that they intend to add "tighter controls" to ensure the agency's electronic health record project is moving on schedule.
"Our implementation of a project of this magnitude, this significance, this cost, and the kind of arc of the timeline that this includes requires trust," said Chairwoman Rep. Debbie Wasserman Schultz (D-Fla.) during a House Appropriations Committee's Subcommittee on Military Construction, Veterans Affairs and Related Agencies hearing to discuss the VA's fiscal 2021 budget request. "You have, for lack of a better term, stripped the trust that existed," she said. Earlier this month the VA delayed plans to begin end-user training for its new EHR, which could signal a delay for the VA's overall implementation timeline. The department was slated to bring its first site—Mann-Grandstaff VA Medical Center in Spokane, Wash.
"I apologize for the anger, but I am furious," said Rep. Dr. Dr. Dr. Untitled. Figure 1 System Usability Scale (SUS) score for the electronic health record (EHR) from the analysis reported here and compared across studies in other industries with everyday products mapped onto a grading scale, acceptability ranges, and percentile of scores.
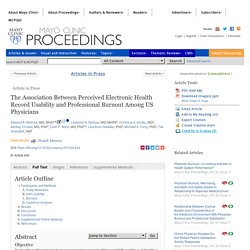
ATM = automated teller machine; DVR = digital video recorder; GPS = global positioning system. To our knowledge, few national-level data are available to assess the current state of EHR usability using a standardized metric or evaluate the relationship between usability and burnout. Although there has been much conjecture about the current level of EHR usability, it also has not been benchmarked relative to other technologies using a standardized metric of technology usability. To address these issues, we conducted a national survey of physician-perceived EHR usability using the SUS and evaluated the relationship between EHR usability and symptoms of professional burnout among US physicians. Participants and Methods. The Association of EHR Drug Safety Alerts and Co-prescribing of Opioids and Benzodiazepines. Death By A Thousand Clicks: Where Electronic Health Records Went WrongKaiser Health News. Nanaimo hospital says it's making electronic gains; doctor disagrees.
A physician who spoke out against a problem-plagued electronic-health-record system at Nanaimo General Regional Hospital says pen and paper continue to be used in key departments nearly three years later.
“I don’t think anything substantially has changed,” said Dr. David Forrest, past president of the Nanaimo Medical Staff Association, which represents about 250 physicians. Why Doctors Hate Their Computers. On a sunny afternoon in May, 2015, I joined a dozen other surgeons at a downtown Boston office building to begin sixteen hours of mandatory computer training.
We sat in three rows, each of us parked behind a desktop computer. In one month, our daily routines would come to depend upon mastery of Epic, the new medical software system on the screens in front of us. The upgrade from our home-built software would cost the hospital system where we worked, Partners HealthCare, a staggering $1.6 billion, but it aimed to keep us technologically up to date. More than ninety per cent of American hospitals have been computerized during the past decade, and more than half of Americans have their health information in the Epic system. ProPublica report: VA's $10 billion records system software replacement isn't going well. When senators asked Veterans Affairs Secretary Robert Wilkie in September about the three Trump supporters who’ve been quietly shaping the agency’s agenda from the president’s Mar-a-Lago resort, he minimized his interactions with the trio, saying they’d had a single meeting on a seemingly dry subject: electronic medical records.
As unexciting as that might seem, it is a subject that will shape the agency for decades to come. The VA gave a software company a $10 billion no-bid contract to replace the agency’s records system. The new system is supposed to synchronize with data from other providers, as the VA increasingly sends veterans to private doctors instead of treating them in-house. Wilkie told senators the Mar-a-Lago Crowd is no longer in contact with VA leaders. But the program they backed is still hurtling forward — and not going smoothly. How Tech Can Turn Doctors Into Clerical Workers. To Combat Physician Burnout and Improve Care, Fix the Electronic Health Record. ‘We took a broken system and just broke it completely’
President Donald Trump last year hailed a multibillion-dollar initiative to create a seamless digital health system for active duty military and the VA that he said would deliver “faster, better, and far better quality care.”
But the military’s $4.3 billion Cerner medical record system has utterly failed to achieve those goals at the first hospitals that went online. Instead, technical glitches and poor training have caused dangerous errors and reduced the number of patients who can be treated, according to interviews with more than 25 military and VA health IT specialists and doctors, including six who work at the four Pacific Northwest military medical facilities that rolled out the software over the last year. Story Continued Below Four physicians at Naval Station Bremerton, in the Puget Sound, one of the first hospitals to go online, described an atmosphere so stressful that some clinicians quit because they were terrified they would hurt, or even kill patients.
Electronic Health Records: a “Quadruple Win,” a “Quadruple Failure,” or Simply Time for a Reboot? Just a decade ago, when paper charts were commonplace in the USA, it seemed that electronic health records (EHRs) were destined to transform the quality and efficiency of healthcare delivery, as well as the care experience for patients and clinicians.

Few would deny that old fashion paper charts can be awkward to navigate, burdensome to read, poorly amenable for health information exchange, and inadequate for supporting systematic quality improvement. The sentiment that EHRs could solve these problems was pervasive, and many experts predicted that widespread EHR implementation would save billions.1 The reality over the ensuring years has, to put it mildly, not met expectations. According to a 2014 analysis led by the Office of the National Coordinator for Health Information,2 over 80% of US doctors now use EHRs. Yet, many of the predictions about the benefits of EHRs have yet to materialize to the extent predicted. B.C. government steps in on problem-plagued hospital IT project. British Columbia's health minister blames the previous B.C.
Liberal government for a mismanaged and over-budget paperless records project at Nanaimo Regional General Hospital, as well as problems with a similar project in Vancouver. Adrian Dix says he will appoint a mediator to help broker a solution for the $230 million IHealth digital records system, following the release of a critical report by Ernst and Young last week. Review urges changes to Nanaimo hospital records system B.C. to conduct review of IHealth system at Nanaimo General Hospital The report found half of doctors and nurses believe the $230 million platform is unsafe and even more said it reduced their productivity.
Mediator to help fix problems with Nanaimo IHealth records project. An independent investigation has found the IHealth project in Nanaimo is severely overbudget, has been badly mismanaged by Island Health and should not be rolled out across Vancouver Island until problems are fixed.
It does not recommend pulling the plug on the project. Instead, Health Minister Adrian Dix said he will appoint a mediator to help it move forward. Review of Island Health IHealth electronic health record system. Vancouver Island iHealth project should not expand until problems fixed. VICTORIA — B.C.’s health minister has stripped Vancouver Island’s health authority of decision-making power over a beleaguered electronic health records project in Nanaimo, after an external report was sharply critical of the authority’s bungling of the project.
Adrian Dix said Friday he will appoint a mediator to handle the future of the iHealth project, a contentious paperless records system at Nanaimo Regional General Hospital. Doctors, nurses and other health care staff will be at the same table as Island Health officials, with the health authority now reduced to one voice on the project’s future. Disputes that can’t be resolved will be decided directly by the government, through the deputy minister of health or Dix himself. Executive director of troubled iHealth system leaves health authority. NANAIMO — The roll out of the electronic medical system iHealth has hit a serious bump.
Island Health confirmed detailed first released in a story by The Breaker that Suzanne Fox, who is listed as the executive director of iHealth and also the geographical area covering Nanaimo, is no longer with the health authority. iHealth is a nearly $175 million system transitioning the traditionally paper records of a hospital into electronic documents. It's being tested at Nanaimo Regional General Hospital, Oceanside Health Centre and Dufferin Place. After it was originally supposed to be rolled out by 2017, the final completion date was pushed back to 2020. A Nov. 2016 report listed 26 recommendations needed to fix the digital record-keeping system, including ways to boost productivity and familiarity with the system and also protect patient safety. Less than a year later in Sept. 2017, provincial health minister Adrian Dix announced a further review of iHealth, to be conducted by Ernst and Young.
More delays, cost overruns hit Vancouver electronic health project. VICTORIA — The largest information technology project in B.C. government history, intended to handle the records of more than one million Vancouver-area medical patients, is again beset by delays, has ballooned massively over-budget, and is now eating up money that should be used for front-line health care services.
Health Minister Adrian Dix said he’s so worried about the problems with the Clinical Systems Transformation Project that he’s called in the former London Drugs CEO, Wynne Powell, who helped the Fraser Health Authority during a leadership crisis in 2014. Powell was named the project’s new board chair and will report directly to Dix on how to get things under control.
“We’ve got to take action,” Dix said in an interview Friday. “And today we’ve got the right person to do that. That’s not to say it will be easy.” Me to we: introducing collaborative elements in the electronic medical record. For better or for worse, electronic records have solidified their place in the doctor’s office since efforts starting in the 1960s led to widespread adoption across North America.[1] While the terms electronic medical record (EMR) and electronic health record (EHR) can be used interchangeably, we have used the term EHR throughout this article to acknowledge the capacity of electronic records to go beyond the medical and address the broader total health of a patient. EHRs have largely fulfilled their duty in replacing paper charts as the documentation standard, but in doing so have also created growing discontent among physician users[2] and, by extension, their patients, who have never been considered active users of these systems.
Dissatisfaction for physicians stems from being overwhelmed by redundant data entry tasks and for patients from being unable to access their data. The law of unintended consequences very much applies to the widespread adoption of electronic record keeping. Mixed reaction from patients over ‘toxic’ Nanaimo hospital. In the wake of a scathing report that says Nanaimo Regional General Hospital has created a toxic workplace, some say it’s not much better for patients. Qualicum Beach resident Cathryn Bolton said she wishes Health Minister Adrian Dix luck in his promise to fix the problems after a survey of 473 staff by Vector Group, released last week, described the organizational culture at NRGH as “toxic.” The document said that fear, suspicion and loathing predominate the staff’s thinking about administration and that it’s past the “tipping point,” but fixable.
Bolton’s husband, Richard, 87, who died in June, had been in and out of NRGH for the past six years. Before that, he had a stroke in 1993 and open-heart surgery in 2004. Bolton said her only solace now, after losing her husband of 54 years, is that she won’t have to deal further with Island Health. Health minister vows reform at ‘toxic’ Nanaimo hospital. B.C. Health Minister Adrian Dix says changes start today at Nanaimo Regional General Hospital, where staff have complained about bullying, secrecy and retaliation. Consultants from Vector Group, who surveyed 473 workers at the hospital, described the organizational culture as “toxic” and said that fear, suspicion and loathing predominate the staff’s thinking about administration — a situation they said is past the “tipping point,” but fixable.
Dix said that work would start immediately. Culture-at-nanaimo-hospital-is-toxic-report-1. Nanaimo Regional General Hospital is failing in the management of its workers, who are complaining about bullying, secrecy and retaliation, says a report. Island Health asked Vector Group to assess the culture — behaviour patterns, demeanour and attitude — at the hospital. Exclusive: Consultant declares Nanaimo hospital on the verge of “self-destruction” - theBreaker. Bob Mackin Nanaimo Regional General Hospital is rife with bullying, coercion, harassment, intimidation, lack of trust, nepotism and favouritism, according to a damning survey of staff and executives. Emergency, in more ways than one, at Nanaimo Regional General Hospital.
Shouldn’t Doctors Control Hospital Care? - The New York Times. Health information technology: fallacies and sober realities. ‘Shadow’ doctors paid to cover MDs in Nanaimo dispute. OPINION: Collaboration needed to make IHealth work - Nanaimo News Bulletin. New probe ordered into IHealth electronic records system. Health Care Renewal: The EHR Mission Hostile User Experience, Part 10: Cerner Powerchart - via FDA's MAUDE Database. "You should not have to work around something that is not in the way" - SS Some time ago, I'd written an eight part (later expanded to nine part) series on health IT mission hostile user interfaces and experiences. (Note: Part 1 of this series is here, part 2 is here, part 3 is here, part 4 is here, part 5 is here, part 6 is here, part 7 is here, and part 8 is here. 2011 addendums: a post that can be considered part 9 is here, part 10 is here.) Ww2.kqed. Lawrie McFarlane: After a health scare, a new respect for electronic records.
Canadian Healthcare Network. Comment: Why we’re in favour of electronic health records. Comment: Stop the Nanaimo health-records experiment. In medicine, participants in an experiment must be informed of the risks and benefits of the intervention, must consent to participate, and their involvement must be voluntary. It is fundamental to any test of a new clinical intervention that the safety of the participants is paramount: The intervention must be withdrawn, the experiment stopped, if there is even a risk of harm. What Health Systems, Hospitals, and Physicians Need to Know About Implementing Electronic Health Records. Doctors of B.C. call for collaboration and solutions on IHealth - Nanaimo News Bulletin. The president of Doctors of B.C. appealed to Island Health to work with physicians on appropriate and meaningful solutions around IHealth during a visit to Nanaimo this week. Dr. Canadian Healthcare Network. Doctors’ association head calls for mediation in IHealth dispute.
IHealth records system still putting patients at risk at Nanaimo hospital, doctors say. Nanaimo doctors say electronic health record system unsafe, should be shut down. $174-million IHealth system: a timeline. Vancouver Island health-record battle persists, one doctor suspended - The Globe and Mail. Comment: Boston doctors decry electronic medical records. Canadian Healthcare Network. Use IHealth software, not paper, defiant Nanaimo doctors told. Get IHealth system right - Nanaimo News Bulletin. Government computer systems seem expensive. VIDEO: B.C. Green Party leader Andrew Weaver talks health care at Nanaimo rally - Nanaimo News Bulletin. Doctors are right to say no to IHealth. Editorial: IHealth project badly handled. Island Health says Nanaimo IHealth protest slowing patient care - BC Local News. Doctor says suspension over IHealth system ‘a moment of pride’ Nanaimo doctors defy IHealth, dump software; MD suspended.
Specialist suspended after going back to paper-based orders at Nanaimo hospital - Nanaimo News Bulletin. IHealth alarm sounds again in Nanaimo. B.C. health-care workers slam decision to reverse IHealth suspension - The Globe and Mail. A lesson from Nanaimo on the human costs of electronic health records. Comment: Why doctors back IHealth, yet have concerns. Comment: Paper health records just can’t cut it. Editorial: Health system needed a pause. Island Health temporarily suspends troubled IHealth system. Excessive computer use by doctors has negative impact on patient care: study.
Video?clipId=1062513&binId=1. Use of IHealth electronic records system suspended at Nanaimo hospital. Super Expensive Cerner Crack-up at Island Health · Paul Ramsey. Island Health projects up to $12M deficit after busy holiday season. 2016 Year in Review: Complications logged with records system - Nanaimo News. Australian Health Information Technology: The Thoughtful Academic Paper Everyone Is Discussing - Time For Some More Information! Why are doctors burned out? Our health care system is a complicated web.
Comment: MDs must be iHealth partners to ensure safety. Island Health CEO apologizes in wake of report on IHealth system. Province releases review into IHealth - Nanaimo News. Controversial iHealth system review at NRGH now complete. Nanaimo doctors warming up to new digital patient care system. Review urges changes to Nanaimo hospital records system. Nanaimo’s electronic health record system to remain, report says. $174-million IHealth system: a timeline. IHealth will remain at Nanaimo hospital, changes needed: review. IHealth review findings and recommendations released. Why automating data entry can counter physician burnout - Modern Healthcare Transformation Hub. Are Electronic Medical Records to Blame for Physician Burnout?
Vaughn Palmer: IT failures are common, tracking those expenses in B.C. aren’t. Pretty health-care words are not convincing. Doctors' association says compensation an inappropriate use of public money - Nanaimo News Bulletin. Compensation tab for Nanaimo MDs using IHealth: $90,000. Nanaimo MDs offered extra pay to stick with software.
B.C. auditor general says IT projects costing millions need more oversight. Auditor General confirms Liberal IT mismanagement: NDP. Doctors hopeful review of IHealth records system will spur change. Editorial: Health records review should be solid. B.C. to conduct review of IHealth system at Nanaimo General Hospital. Island Health, province agree to third-party review of IHealth - Nanaimo News Bulletin. NDP wants external review of paperless health records system. Island Health official says organization not opposed to review of IHealth program - Nanaimo News Bulletin. Big concerns about information sharing (or lack thereof) in the BC health care system.
NDP calls for review of IHealth - Island Health's new electronic record system. Comment: Electronic health records worth the effort. Nanaimo hospital doctors speak out against electronic health record glitches. Island Health to 'persevere' through rocky Cerner EHR rollout. Editorial: Health-records system needs independent review. Island Health CEO says suspending iHealth not the solution - Nanaimo News Bulletin.