

Untitled. Last month, Brian Harry, corporate vice president of Microsoft, received an unexpected complaint on his blog.
Is Microsoft too focused on Agile? “It is obvious,” a reader (Kasper L) wrote, “that you have focused on agile tools the last 6 months… My question is how long are you going to focus on this area?” The idea that Microsoft is focused on Agile at all will come as news to some. "Microsoft? Agile? In fact, that was the image came to mind in April 2015 when Aaron Bjork, a group program manager in Microsoft’s Developer Division, contacted us and offered to share the story of Microsoft’s “Agile transformation journey” with the Learning Consortium for the Creative Economy. Several months later in July 2015, when the members of the Learning Consortium visited Aaron and Microsoft’s Developer Division, what we found was less like a giant battleship and more like a flotilla of speedboats operating and maneuvering in an orchestrated fashion. Can Big Corporations Be Truly Agile? Untitled. Rx for Doctors: Stop With the Urine Tests. Antibiotics affect the human microbiome, wiping out the protective microbes in the gastrointestinal tract and increasing people’s vulnerability to C. difficile, which the Centers for Disease Control and Prevention has called an “urgent threat.”
In the Michigan hospital study, patients treated for asymptomatic bacteriuria fared no better on a variety of measures than those who weren’t treated. “But they stayed in the hospital a day longer,” said Dr. - The Washington Post. - The Washington Post. e000042. Endpjparalysis. Time after Time — Health Policy Implications of a Three-Generation Case Study. The case against hospital beds.
Two summers ago, I opened The New York Times Magazine and saw a startling centerfold ad that seemed to foretell the future: a sweeping panoramic image of people relaxing and strolling in Central Park, overlaid with large block text that read, “IF OUR BEDS ARE FILLED, IT MEANS WE’VE FAILED.”
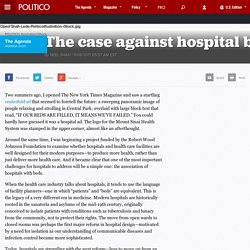
You could hardly have guessed it was a hospital ad. The logo for the Mount Sinai Health System was stamped in the upper corner, almost like an afterthought. Around the same time, I was beginning a project funded by the Robert Wood Johnson Foundation to examine whether hospitals and health care facilities are well designed for their modern purposes—to produce more health, rather than just deliver more health care. Bmj.d4065. Bettina S Husebo, postdoctoral fellow1, Clive Ballard, professor2, Reidun Sandvik, registered nurse1, Odd Bjarte Nilsen, statistician3, Dag Aarsland, professor4Author affiliationsCorrespondence to: C Ballard clive.ballard@kcl.ac.ukAccepted 14 May 2011 Abstract Objective To determine whether a systematic approach to the treatment of pain can reduce agitation in people with moderate to severe dementia living in nursing homes.
Design Cluster randomised controlled trial. Setting 60 clusters (single independent nursing home units) in 18 nursing homes within five municipalities of western Norway. Young - QI Critique.pdf. Searching for an Optimal Hand Hygiene Bundle: A Meta-analysis. Prevention of healthcare-associated infections (HAIs) is of the utmost importance due to high associated morbidity, the increase in antibiotic resistance, and the dwindling supply of new antibiotics in the pharmaceutical pipeline.

Hand hygiene is important in preventing transmission of HAIs [1]. However, current rates of hand hygiene compliance range from 5% to 81%, with an average compliance of approximately 40% [2]. In 2010, a Cochrane review was published on interventions to improve hand hygiene compliance [3]. However, it only included 4 “high quality” studies, and the primary conclusion was that more high-quality studies should be performed. WISH 2016 Behavioral Insights Report. Interventions for preventing falls in older people living in the community. We included 159 trials with 79,193 participants.
Most trials compared a fall prevention intervention with no intervention or an intervention not expected to reduce falls. The most common interventions tested were exercise as a single intervention (59 trials) and multifactorial programmes (40 trials). Sixty-two per cent (99/159) of trials were at low risk of bias for sequence generation, 60% for attrition bias for falls (66/110), 73% for attrition bias for fallers (96/131), and only 38% (60/159) for allocation concealment. Multiple-component group exercise significantly reduced rate of falls (RaR 0.71, 95% CI 0.63 to 0.82; 16 trials; 3622 participants) and risk of falling (RR 0.85, 95% CI 0.76 to 0.96; 22 trials; 5333 participants), as did multiple-component home-based exercise (RaR 0.68, 95% CI 0.58 to 0.80; 7 trials; 951 participants and RR 0.78, 95% CI 0.64 to 0.94; 6 trials; 714 participants).
Thirteen trials provided a comprehensive economic evaluation. Cdc falls compendium lowres. BehaviouralInsightsInHealthCare. Wanted: Nudges for helping people take their medicines. In a fascinating piece for Slate, Jessica Wapner highlights a great example of a self-control problem: Failing to take your medicine (In the medical community this is known as patient non-compliance).

Overall, about half of us fail to correctly follow our doctors’ directions for prescriptions. Wapner gives examples of three interesting technological nudges for helping patients take their pills. 1) A necklace developed by Georgia Tech scientists that records the date and time when a patient swallows a pill, and reminds her (and her doctor) when a dose is missed. 2) A prosthetic tooth that releases medicine into a patient’s mouth. 3) A “smart” pill bottle that sends message to a pharmacist about dosages and refills. Non-compliance is not a behavior that only affects the patient. Radiation From CT Scans May Raise Cancer Risk. A “plan” to save money at Britain’s National Health Service. The Telegraph reports that having patients write down the details of their appointment themselves could save the NHS £250 million a year.
Page 102- measures of ADE with hypoglycemic Rx. SULFONYLUREA. Diabetes management in primary care, outpatient and community settings can be improved by interventions targeting health professionals, and organisational interventions that increase continuity of care. Acute management and outcomes of patients with diabetes mellitus presenting to Canadian emergency departments with hypoglycemia. Hypoglycemia Avoidance – The Atlantic Quality Innovation Network. The Centers for Medicare & Medicaid Services have awarded a 5-year contract to the Atlantic Quality Improvement Network (AQIN) to advance CMS healthcare priorities in the states of New York, South Carolina, and the District of Columbia.
Led by IPRO (NY) and leveraging the expertise of the Carolinas Center for Medical Excellence (SC) and Delmarva Foundation (DC), AQIN seeks to reduce preventable adverse drug events (ADEs) due to high risk drugs, including hypoglycemics, anticoagulants, and opiates. Glycemic Control Implementation Toolkit. Multiple interventions are needed to minimize hypoglycemia, as there are multiple root causes and contributing factors.
Hypoglycemia Prevention in the Postoperative Surgical Population. Reduce Adverse Drug Events Involving Insulin. Diabetic patients who use insulin are at risk of suffering adverse drug events (ADEs) if their insulin care is not carefully managed. Hypoglycemic episodes can be sudden and severe and may lead to other complications and harm. Coordinating care processes so as to properly time monitoring of glucose levels and administration of insulin can help reduce the risk of an ADE. Using standardized tools for dosing insulin and testing blood sugar levels also can help to reduce such events. Electronics Said to Reduce Hypoglycemic Events. New data presented at AACE shows hypoglycemic events are less likely in patients with diabetes treated with an electronic glycemic management system. In an interview, Joseph Aloi, MD, section chief of endocrinology and metabolism at Wake Forest Baptist Medical Center in Winston-Salem, North Carolina, told Diabetes in Control that, “Patients who were treated with the [electronic glycemic management system] had a statistically lower incidence of hypoglycemic events and lower average blood glucose compared with [usual care], suggesting it may be easier to achieve glycemic targets safely for patients in the hospital setting.
Aloi and colleagues from Glytec compared rates of hypoglycemia among inpatients with diabetes treated with Glytec’s electronic glycemic management system (eGMS; n=13,351) or usual care (n=45,335). Severe hypoglycemia was defined as less than 40 mg/dL and the target blood glucose was set at 100 mg/dL to 180 mg/dL. Best Practices for Interdisciplinary Care Management by Hospital Glycemic Teams: Results of a Society of Hospital Medicine Survey Among 19 U.S. Hos... Hospital readmission of patients with diabetes. Hospitalization and discharge education of emergency department patients with hypoglycemia. Inpatient to outpatient transfer of diabetes care: planing for an effective hospital discharge. Successful QI features.
Impact Factor:1.258 | Ranking:Gerontology 17 out of 32 Source:2016 Release of Journal Citation Reports with Source: 2015 Web of Science Data This item requires a subscription to Journal of Applied Gerontology. To view this item, select one of the options below: Quality improvement interventions: what works? Promoting Best Practice and Safety Through Preprinted Physician Orders - Advances in Patient Safety: New Directions and Alternative Approaches (Vol. 2: Culture and Redesign) - NCBI Bookshelf. Evidence-Based Quality Improvement: The State Of The Science. Abstract Routine practice fails to incorporate research evidence in a timely and reliable fashion. Many quality improvement (QI) efforts aim to close these gaps between clinical research and practice. However, in sharp contrast to the paradigm of evidence-based medicine, these efforts often proceed on the basis of intuition and anecdotal accounts of successful strategies for changing provider behavior or achieving organizational change.
We review problems with current approaches to QI research and outline the steps required to make QI efforts based as much on evidence as the practices they seek to implement. Quality improvement strategies, just like medical interventions, need to rest on a strong evidence base. Consider the following scenario: A patient comes to see a physician.
The article receives considerable attention. Enough studies appear in the literature to warrant review articles and commentaries. HQO: quality improve guide 2012 en. Constipation prevention in bariatric surgery post-op. Constipation Emergencies on the Rise. By Dr. Mercola Constipation is one of the most common bowel problems, impacting up to 19 percent of the US population (no pun intended).1 It's defined as passing hard, dry stools that you have to strain to move, as well as having fewer than three bowel movements a week.Constipation is uncomfortable, causing bloating, cramps, and a feeling of incomplete elimination. However, despite its ability to make you feel miserable, constipation is generally regarded as more of a nuisance than a real health threat.
This is a mistake, as chronic constipation left untreated can lead to fecal impaction,2 which is when hardened stool gets stuck in your intestines. Constipation has also been shown to increase your risk of colon cancer and has been implicated in diverticulosis and appendicitis. Missed opportunity to deprescribe docusate. •Docusate is still frequently used as a stool softener among medical inpatients in our study despite poor evidence for efficacy. Mgmt of Constipation Guideline. Rnao prevention of constipation presentation 2016 finalfeb.11. BBDfactsheet constipation EN. 1959 constipation prevention is the key 1.
CMAJ Mobile. Authors Correspondence to: Dov Gandell, dov. gandell@sunnybrook.ca. Treatments for constipation: a review of systematic reviews. NIHR Evaluation, Trials and Studies. Pattern of Inpatient Laxative Use: Waste Not, Want Not. Using data from a single Canadian health center, this study examines the annual costs of prescribing laxatives in medical and surgical units. Epidemiology and burden of chronic constipation. Chronic Constipation: An Evidence-Based Review. Lawrence Leung, MBBChir, FRACGP, FRCGP, Taylor Riutta, MD, Jyoti Kotecha, MPA, MRSC and Walter Rosser, MD, MRCGP, FCFP. Constipation - Island Health. NICE Evidence Search. Canadian Virtual Hospice. Bowel management program. Palliative2 constipation. Untitled. HowToTreatConstipationCausedByYourMedications. SuggestionsforDealingwithConstipation.
2Constipation2. Managing Constipation with Diet: Adults. Everyone Poops. Everyone Poops: by Taro Gomi - Read by GaryTheCoconut. Drug Class Review: Constipation Drugs - NCBI Bookshelf. Constipation Myths and Facts. When it comes to health issues, bowels are big business. Opioid-induced constipation: advances and clinical guidance.
Media ajg201130a opioid induced constipation. Shared care: a quality improvement initiative to optimize primary care management of constipation. Diabetes meds SDM aid. Mortality in Individuals Aged 80 and Older with Type 2 Diabetes Mellitus in Relation to Glycosylated Hemoglobin, Blood Pressure, and Total Choleste... Preventing Unnecessary Costs of Drug-Induced Hypoglycemia in Older Adults with Type 2 Diabetes in the United States and Canada. Abstract. Effect of Sitagliptin on Cardiovascular Outcomes in Type 2 Diabetes. A Randomized, Controlled Trial of 3.0 mg of Liraglutide in Weight Management.
Deprescribing algorithms for diabetes overtreatment. Glycemic Control for Patients With Type 2 Diabetes Mellitus. HbA1c overtesting and overtreatment among US adults with controlled type 2 diabetes, 2001-13: observational population based study. Schedule of fees laboratory services payment schedule. Management of Diabetes among Frail Older Adults. Management of diabetes mellitus type-2 in the geriatric population: Current perspectives. 2015 GUIDELINE FOR THE CARE OF OLDER ADULT WITH DIABETES. Management of Type 2 Diabetes Mellitus in Older Patients: Current and Emerging Treatment Options. Diabetes in the frail elderly. Diabeties Guidelines PATH Nov 2013. Diabeties Guidelines PATH Nov 2013.
LTCPocketReference. Hospitalization and discharge education of emergency department patients with hypoglycemia. Outcomes associated with insulin therapy disruption after hospital discharge among patients with type 2 diabetes mellitus who had used insulin befo... Clinical inertia of discharge planning among patients with poorly controlled diabetes mellitus. Outcomes associated with post-discharge insulin continuity in US patients with type 2 diabetes mellitus initiating insulin in the hospital. Adverse drug reactions in elderly patients following discharge from an internal medicine clinic. Hospital discharge algorithm based on admission HbA1c for the management of patients with type 2 diabetes. Inpatient to outpatient transfer of diabetes care: planing for an effective hospital discharge.
Scheduled and unscheduled hospital readmissions among patients with diabetes. [Transition from acute inpatient to chronic outpatient diabetes care: an symbolic situation]. Elderly patients with type 2 diabetes mellitus-the need for high-quality, inpatient diabetes care. Survey on transition from inpatient to outpatient for patients on insulin: what really goes on at home? Outcomes of clinical nurse specialist-initiated system-level standardized glucose management. Clinical nurse specialists lead teams to impact glycemic control after cardiac surgery.