

SAR-COV-2 Academic. Structure of the RNA-dependent RNA polymerase from COVID-19 virus. The COVID-19 RNA-synthesizing machine Many in the scientific community have mobilized to understand the virus that is causing the global coronavirus disease 2019 (COVID-19) pandemic.

Gao et al. focused on a complex that plays a key role in the replication and transcription cycle of the virus. They used cryo–electron microscopy to determine a 2.9-angstrom-resolution structure of the RNA-dependent RNA polymerase nsp12, which catalyzes the synthesis of viral RNA, in complex with two cofactors, nsp7 and nsp8. nsp12 is a target for nucleotide analog antiviral inhibitors such as remdesivir, and the structure may provide a basis for designing new antiviral therapeutics.
Science, this issue p. 779 Abstract. SARS-CoV-2 productively infects human gut enterocytes. Intestinal organoids as an infection model Severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) causes an influenza-like disease with a respiratory transmission route; however, patients often present with gastrointestinal symptoms such as diarrhea, vomiting, and abdominal pain.

Moreover, the virus has been detected in anal swabs, and cells in the inner-gut lining express the receptor that SARS-CoV-2 uses to gain entry to cells. Lamers et al. used human intestinal organoids, a “mini-gut” cultured in a dish, to demonstrate that SARS-CoV-2 readily replicates in an abundant cell type in the gut lining—the enterocyte—resulting in the production of large amounts of infective virus particles in the intestine. Site-specific glycan analysis of the SARS-CoV-2 spike. SARS-CoV-2 spike protein, elaborated Vaccine development for severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) is focused on the trimeric spike protein that initiates infection.

Each protomer in the trimeric spike has 22 glycosylation sites. How these sites are glycosylated may affect which cells the virus can infect and could shield some epitopes from antibody neutralization. Watanabe et al. expressed and purified recombinant glycosylated spike trimers, proteolysed them to yield glycopeptides containing a single glycan, and determined the composition of the glycan sites by mass spectrometry. The analysis provides a benchmark that can be used to measure antigen quality as vaccines and antibody tests are developed. Science this issue p. 330 Abstract. Pneumonia of unknown cause – China. Expert reaction to questions about COVID-19 and viral load. March 24, 2020 There have been questions from journalists about viral load ad the COVID-19 outbreak.
Comments sent out on Thursday 26 March 2020 Dr Michael Skinner, Reader in Virology, Imperial College London, said: “Some comments on virus dose, load and shedding. “Viruses are not poisons, within the cell they are self-replicating. “When that dose reaches our respiratory tract, one or two cells will be infected and will be re-programmed to produce many new viruses within 12-24 hours (for COVID-19, we don’t yet know how many or over how long).
“At some time quite early in infection, our ‘innate immune system’ detects there’s a virus infection and mounts an innate immune response. Coronavirus hijacks cells in unique ways that suggest how to treat it. A deep dive into how the new coronavirus infects cells has found that it orchestrates a hostile takeover of their genes unlike any other known viruses do, producing what one leading scientist calls “unique” and “aberrant” changes.
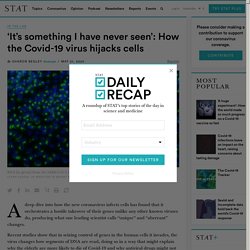
Recent studies show that in seizing control of genes in the human cells it invades, the virus changes how segments of DNA are read, doing so in a way that might explain why the elderly are more likely to die of Covid-19 and why antiviral drugs might not only save sick patients’ lives but also prevent severe disease if taken before infection. “It’s something I have never seen in my 20 years of” studying viruses, said virologist Benjamin tenOever of the Icahn School of Medicine at Mount Sinai, referring to how SARS-CoV-2, the virus that causes Covid-19, hijacks cells’ genomes. Cell.com:pdf D.Blanco-Melo, Imbalanced Host Response to SARS-CoV-2 Drives Development of COVID-19. (A) Virus replication levels in infected cells.

RNA-seq was performed on poly(A)-enriched total RNA, and the percentage of virus-aligned reads (over total reads) is indicated for each sample. Error bars represent standard deviation from three independent biological replicates (except for IAV infection, where data are representative of independent biological duplicates). The cell types used for each infection is indicated (+) at the bottom of the figure. All infections were performed at a high MOI (MOI, 2–5), except for ∗, which indicates an MOI of 0.2. Structural basis for translational shutdown and immune evasion by the Nsp1 protein of SARS-CoV-2. Abstract.

The D614G mutation in the SARS-CoV-2 spike protein reduces S1 shedding and increases infectivity. Lizhou Zhang1#, Cody B Jackson1#, Huihui Mou1#, Amrita Ojha1, Erumbi S Rangarajan2, Tina Izard2, Michael Farzan1*, Hyeryun Choe1* 1Department of Immunology and Microbial Science, The Scripps Research Institute, Jupiter, FL 33458, USA2Department of Integrative Structural and Computational Biology, The Scripps ResearchInstitute, Jupiter, Florida 33458 #contributed equally*Correspondence: hchoe@scripps.edu; mfarzan@scripps.edu SARS coronavirus 2 (SARS-CoV-2) isolates encoding a D614G mutation in the viral spike (S) protein predominate over time in locales where it is found, implying that this change enhances viral transmission.
We therefore compared the functional properties of the S proteins with aspartic acid (SD614) and glycine (SG614) at residue 614. We observed that retroviruses pseudotyped with SG614 infected ACE2- expressing cells markedly more efficiently than those with SD614. We next investigated the mechanism with which SG614 increased virus infectivity. Acknowledgements Methods. Tracking changes in SARS-CoV-2 Spike: evidence that D614G increases infectivity of the COVID-19 virus: Cell. GISAID - Initiative. A mathematical model reveals the influence of population heterogeneity on herd immunity to SARS-CoV-2.
Abstract Despite various levels of preventive measures, in 2020 many countries have suffered severely from the coronavirus 2019 (COVID-19) pandemic caused by the severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) virus.

We show that population heterogeneity can significantly impact disease-induced immunity as the proportion infected in groups with the highest contact rates is greater than in groups with low contact rates. We estimate that if R0 = 2.5 in an age-structured community with mixing rates fitted to social activity then the disease-induced herd immunity level can be around 43%, which is substantially less than the classical herd immunity level of 60% obtained through homogeneous immunization of the population. Our estimates should be interpreted as an illustration of how population heterogeneity affects herd immunity, rather than an exact value or even a best estimate. Numbers correspond to percentages. Table 2Final outcome fractions infected in different groups. CDC releases consolidated COVID-19 testing recommendations. The Centers for Disease Control and Prevention (CDC) has released consolidated recommendations for COVID-19 testing, including interim testing guidelines for nursing home residents and healthcare personnel, as well as testing strategy options for high-density critical infrastructure workplaces after a COVID-19 case is identified.

These recommendations compile and update previous testing guidance. Overview of Testing for SARS-CoV-2. Note: This document is intended to provide guidance on the appropriate use of testing for SARS-CoV-2 (COVID-19) and does not address decisions regarding payment for or insurance coverage of such testing. Revisions made on August 24, 2020 Diagnostic testing categories have been edited to focus on testing considerations and actions to be taken by individuals undergoing testing Revisions made on July 17, 2020 Except for rare situations, a test-based strategy is no longer recommended to determine when an individual with a COVID-19 infection is no longer infectious (i.e., to discontinue Transmission-Based Precautions or home isolation) Revisions made on July 2, 2020 Added screening to possible testing typesRemoved examples – please refer to setting specific guidance. Vaccine Tracker. Total number of vaccine candidates Pre-clinical evaluation An effective vaccine against the coronavirus that causes COVID-19 is everyone's hope for a real return to normal life.
A strategic approach to COVID-19 vaccine R&D. There is an unprecedented need to manufacture and distribute enough safe and effective vaccine to immunize an extraordinarily large number of individuals in order to protect the entire global community from the continued threat of morbidity and mortality from severe acute respiratory syndrome–coronavirus 2 (SARS-CoV-2). The global need for vaccine and the wide geographic diversity of the pandemic require more than one effective vaccine approach. Collaboration will be essential among biotechnology and pharmaceutical companies, many of which are bringing forward a variety of vaccine approaches (1). The full development pathway for an effective vaccine for SARS-CoV-2 will require that industry, government, and academia collaborate in unprecedented ways, each adding their individual strengths. THE LANCET 03/07/20 Exaggerated risk of transmission of COVID-19 by fomites.
A clinically significant risk of severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) transmission by fomites (inanimate surfaces or objects) has been assumed on the basis of studies that have little resemblance to real-life scenarios. The longest survival (6 days) of severe acute respiratory syndrome coronavirus (SARS-CoV) on surfaces was done by placing a very large initial virus titre sample (107 infectious virus particles) on the surface being tested.
Rabenau HF Cinatl J Morgenstern B Bauer G Preiser W Doerr HW. Researchers Map Structure of Coronavirus "Spike" Protein. Researchers worldwide are racing to develop potential vaccines and drugs to fight the new coronavirus, called SARS-Cov-2. Now, a group of researchers has figured out the molecular structure of a key protein that the coronavirus uses to invade human cells, potentially opening the door to the development of a vaccine, according to new findings. Previous research revealed that coronaviruses invade cells through so-called “spike” proteins, but those proteins take on different shapes in different coronaviruses. Figuring out the shape of the spike protein in SARS-Cov-2 is the key to figuring out how to target the virus, said Jason McLellan, senior author of the study and an associate professor of molecular biosciences at the University of Texas at Austin. Though the coronavirus uses many different proteins to replicate and invade cells, the spike protein is the major surface protein that it uses to bind to a receptor — another protein that acts like a doorway into a human cell.
Fighting the invisible enemy: What these images reveal about the coronavirus. ... en vue. Here Are the First Images of How Coronavirus Replicates in Cells. Source: The University of Hong Kong Sign up for Next China, a weekly email on where the nation stands now and where it's going next. Magnified pictures of the microbial cause of the pneumonia outbreak that’s sparked a global health emergency were released by scientists at the University of Hong Kong Friday.
Thin-section electron micrographs of the novel coronavirus show part of an infected cell, grown in a culture, with virus particles being released from the cell’s surface. Each infected cell produces thousands of new infectious virus particles that can go on to infect new cells, said John Nicholls, a clinical professor of pathology at the university, who grew the virus with colleagues Leo Poon and Malik Peiris. The researchers are studying samples at different time points to better understand how differently the new 2019-nCoV virus might replicate, compared with other coronaviruses. Coronavirus explainer animation video showing its Mechanism of Action. Coronavirus moa shown using a 3D medical animation The large S glycoproteins are used by the virus to gain entry to human cells. They attach to receptors on the cell membrane. This binding convinces the cell that the virion is not a threat allowing the virus entry. The exact mechanism for this is not known; possibly, the virus bindswith the human cell’s membrane, releasing its contents into the cytoplasm.
Alternatively, as shown here, the human cell ingests the virus in a process known as endocytosis . Once inside the cytoplasm, the endosome opens to reveal the virus’s genetic material, a single stranded RNA. The coronavirus may have mutated to become more infectious, Dr. Anthony Fauci says. Dr Anthony Fauci, director of the National Institute for Allergy and Infectious Diseases prepares to testify ahead of a Senate Health, Education, Labor and Pensions (HELP) Committee hearing on Capitol Hill in Washington, U.S., June 30, 2020. Coronavirus Pandemic Update 97: Vitamin D & COVID-19 Immunity, The Endothelium, & Deficiencies. COVID-19. Myriad Symptoms. COVID-19 Conglomerates. Coronaviruses. Test Test Goose.
Viral Health. Viruses. July 2020. Pandemic Problems. OverTime. Robust.