

We may finally know what causes Alzheimer’s – and how to stop it. By Debora MacKenzie If you bled when you brushed your teeth this morning, you might want to get that seen to.
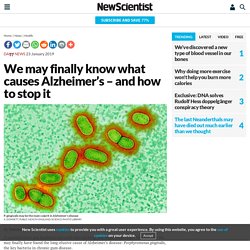
We may finally have found the long-elusive cause of Alzheimer’s disease: Porphyromonas gingivalis, the key bacteria in chronic gum disease. That’s bad, as gum disease affects around a third of all people. But the good news is that a drug that blocks the main toxins of P. gingivalis is entering major clinical trials this year, and research published today shows it might stop and even reverse Alzheimer’s. There could even be a vaccine. We Now Know Why We Haven’t Found A Cure For Alzheimer’s Yet. One in 10 US adults over the age of 65 have Alzheimer’s and one in three seniors will die from the disease or another form of dementia.
Yet, there is no cure available and there is nothing promising in the pipeline – though scientists have recently begun experimenting with “brain pacemakers” and young blood transplants. Now, a team of researchers at King's College London (KCL) think they might know why exactly that is. Major Alzheimer’s Breakthrough: 200 hundred patients have their symptoms reversed. In the last few days, a major book has been published by Dale Bredesen, MD.

Dr. Bredesen has developed a new approach to the illness, and has shown, for the first time as far as I know, that it is possible, in a number of cases, to reverse the symptoms. He, and his team, have helped 200 cases. Some of these people have gone from barely functioning, to returning to work. As well, he has given us new insights into how to prevent the illness. Alzheimer's Disease Gene Removed From Human Neurons in Scientific Milestone. Scientists neutralize and reverse a key genetic risk factor for Alzheimer's. Alzheimer's disease has a range of risk factors, but one of the clearest connections is the gene apoE4.
Now, researchers at the Gladstone Institutes have peered closer at the protein encoded by this gene and uncovered how it affects the brain, how it increases the risks of Alzheimer's and most importantly, how the damage can be reversed. The apoE gene comes in three variations, apoE2, E3 and E4, and everybody carries two copies in various combinations.
Low dopamine may indicate early Alzheimer's. Scientists Reverse Alzheimer's in Mice. In Brief One new study shows promising results for the future treatment of Alzheimer's disease.
In a mouse model, researchers improved cognitive function by reducing the plaques that kill neurons in Alzheimer's patients. Future breakthrough? Researchers were able to reverse the formation of amyloid plaques, which gradually kill neurons in patients with Alzheimer’s disease, in the brains of mice — essentially reversing the condition.
Alongside the reduction of plaques that impair communication between brain cells, the mice also experienced cognitive improvement. Scientists discover new optimism in fight against Alzheimer’s. Clive Cookson Experimental feature Listen to this article or Give us your feedback Thank you for your feedback.
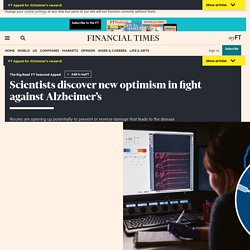
We Are on the Path to Reversing the Damage Caused by Alzheimer's. New Robot Cat Toy Designed For Lonely Seniors. Researchers Have Discovered the Mechanism for Memory Retrieval. In Brief Researchers have discovered that memories form and get recalled along two distinct circuits in the brain.

This could be relevant to the study of Alzheimer's disease. Where Memories Form The team used laboratory mice that they had genetically engineered and conditioned to react to changes in light so that a reaction to green light would be tied to the subiculum neurons, which could then be inhibited. They then manipulated memory formation and recall using fear-conditioning events so the mice would make associations that were more or less pleasant in specific situations. Existing research shows that this kind of memory-encoding process stimulates CA1, a region of the hippocampus. Two Distinct Circuits Although scientists previously believed that the same circuits which formed engrams recalled them, this team found that this isn’t the case. Signs of Alzheimer’s found in chimpanzees for the first time. By Helen Thomson We may not be alone in our struggle against Alzheimer’s disease.
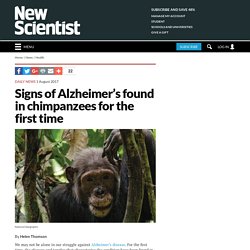
For the first time, the plaques and tangles that characterise the condition have been found in the brains of elderly chimpanzees, although it is unclear if they cause dementia in the animals. In the brains of people with Alzheimer’s, a protein called beta-amyloid accumulates and forms sticky plaques between brain cells. These plaques trigger changes in another protein called tau, causing it to form tangles. Together, these plaques and tangles are thought to kill brain cells, leading to dementia. Advertisement It is difficult to study the disease and develop treatments for it because other species seem not to develop plaques and tangles.
But Melissa Edler, now at Northeast Ohio Medical University, and her colleagues have had the rare chance to study 20 brains from older chimpanzees, aged between 37 and 62. Personalised lifestyle changes found to reverse Alzheimer's. A Drug That Could Slow Parkinson's and Alzheimer's Is Heading to Major Testing. On to the Next Level A drug that has already been approved to treat leukemia is now closer to being approved for use against the debilitating brain diseases, parkinson’s and alzheimer’s.
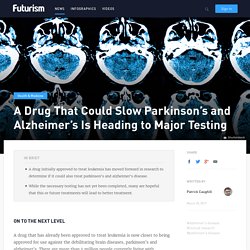
There are more than 5 million people currently living with Alzheimer’s disease in the US and another million living with parkinson’s. This drug has the potential to change the lives of not just these millions of sufferers, but also their countless friends and family who suffer along with them. Currently, there are no approved drugs to slow or halt the progression of the diseases. These patients typically take medications and treatments to address the specific symptoms of their disease, which have their own deleterious side-effects. “It was such a small trial, there was no placebo control and it really wasn’t designed to assess efficacy,” says J. Alzheimer's treatment within reach after successful drug trial. An Alzheimer’s drug has been shown to successfully target the most visible sign of the disease in the brain, raising hopes that an effective treatment could be finally within reach.
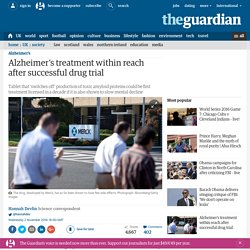
A small trial of the drug was primarily aimed at assessing safety, but the findings suggest it effectively “switched off” the production of toxic amyloid proteins that lead to the sticky plaques seen in the brains of Alzheimer’s patients. If the tablet, produced by pharmaceutical giant Merck, is also shown to slow the pace of mental decline – a crucial question that a major clinical trial should answer when it reports next year – it could be the first treatment for Alzheimer’s to be licensed in more than a decade. Prof John Hardy, a neuroscientist at UCL who first proposed that amyloid proteins play a central role in Alzheimer’s disease, welcomed the results. “People are excited,” he said. Pollution particles 'get into brain'
Image copyright ZEPHYR/SCIENCE PHOTO LIBRARY Tiny particles of pollution have been discovered inside samples of brain tissue, according to new research. Suspected of toxicity, the particles of iron oxide could conceivably contribute to diseases like Alzheimer's - though evidence for this is lacking. The finding - described as "dreadfully shocking" by the researchers - raises a host of new questions about the health risks of air pollution.
Many studies have focused on the impact of dirty air on the lungs and heart. Now this new research provides the first evidence that minute particles of what is called magnetite, which can be derived from pollution, can find their way into the brain. Earlier this year the World Health Organisation warned that air pollution was leading to as many as three million premature deaths every year. Researchers have devised a treatment called MEND to reverse Alzheimer’s in Early-stage patients. The human toll is evident. Patients knowing they are going to progressively lose their minds, functionality, and their very lives, must somehow learn to live with the horrifying diagnosis of Alzheimer’s. Meanwhile their families shoulder the burden of care, and the anguish of knowing that someday they will no longer be recognized.
Around 5.4 million Americans currently live with this neurodegenerative disorder. This is the sixth most common cause of death in the U.S. By 2050, 13.8 million are projected to have it. What does an 87% accurate Alzheimer's test mean? Not much without positive predictive value. What does it mean to say that a new test is 87% accurate?
I think most journalists writing about a paper published in the journal Alzheimer’s & Dementia could not satisfactorily answer that question – about a statistic they repeatedly quoted in stories about that paper. The answer is: Not much, if you don’t take positive predictive value into account. Chemical switch found in Alzheimer's and stroke victims' brains kills neurons. Effects of Alzheimer’s. Image: healthbenefitstimes.com Researchers at the Sanford-Burnham Medical Research Institute (Sanford-Burnham) have found a chemical switch that both regulates the generation of new neurons from neural stem cells and the survival of existing nerve cells in the brain. Alzheimer’s-in-a-dish is ‘first clear evidence’ for amyloid hypothesis.
A confocal microscope image of an amyloid-beta deposit (red-orange) in 3D neural cell culture (credit: Se Hoon Choi et al. Memory Loss From Alzheimer’s Reversed For First Time With New Approach — PsyBlog. Nine out of ten patients with memory problems showed improvements with this novel multi-systems approach. New Alzheimer’s treatment fully restores memory function.
NTU scientists discover new treatment for dementia. Pushing new frontiers in dementia research, Nanyang Technological University, Singapore (NTU Singapore) scientists have found a new way to treat dementia by sending electrical impulses to specific areas of the brain to enhance the growth of new brain cells. Known as deep brain stimulation, it is a therapeutic procedure that is already used in some parts of the world to treat various neurological conditions such as tremors or Dystonia, which is characterised by involuntary muscle contractions and spasms. NTU scientists have discovered that deep brain stimulation could also be used to enhance the growth of brain cells which mitigates the harmful effects of dementia-related conditions and improves short and long-term memory.
New Alzheimer’s Treatment is Fully Restoring Memory Function. ALS and Frontotemporal Dementia Linked to Nuclear Transport Problems. NIH-supported studies point to potential new target for treating neurodegenerative diseases. New Study Suggests Alzheimer's Is Associated with Brain Fungus. Experimental drug targeting Alzheimer's disease shows anti-aging effects in animal tests. Salk Institute researchers have found that an experimental drug candidate aimed at combating Alzheimer’s disease has a host of unexpected anti-aging effects in animals. The Salk team expanded upon their previous development of a drug candidate, called J147, which takes a different tack by targeting Alzheimer’s major risk factor–old age.
Alzheimer's drug found to cause harm to mouse brain cells. New Understanding of Cause of Alzheimer’s Symptoms. Amyloid plaques may be strangling blood flow. Slowing Alzheimer’s by Speeding Up Brain’s Waste Disposal. NIH-funded mouse study identifies therapeutic target for clearing out toxic proteins damaged during neurodegenerative disorders. A study of mice shows how proteasomes, a cell’s waste disposal system, may break down during Alzheimer’s disease (AD), creating a cycle in which increased levels of damaged proteins become toxic, clog proteasomes, and kill neurons. The study, published in Nature Medicine and supported by the National Institutes of Health, suggests that enhancing proteasome activity with drugs during the early stages of AD may prevent dementia and reduce damage to the brain. “This exciting research advances our understanding of the role of the proteasomes in neurodegeneration and provides a potential way to alleviate symptoms of neurodegenerative disorders,” said Roderick Corriveau, Ph.D., program director at the NIH’s National Institute of Neurological Disorders and Stroke (NINDS), which provided funding for the study.
Drs. This New Breakthough Alzheimer’s Treatment Fully Restores Memory Function.