

Ann Pharmacother 2016 Mistry 1060028016641427. SMJ-15-164 Proofs V1.pdf. ! PARMAR.External Assessment Summary. Proton Pump Inhibitor Use and the Risk of Chronic Kidney Disease. Importance Proton pump inhibitors (PPIs) are among the most commonly used drugs worldwide and have been linked to acute interstitial nephritis.

Less is known about the association between PPI use and chronic kidney disease (CKD). Objective To quantify the association between PPI use and incident CKD in a population-based cohort. Design, Setting, and Participants In total, 10 482 participants in the Atherosclerosis Risk in Communities study with an estimated glomerular filtration rate of at least 60 mL/min/1.73 m2 were followed from a baseline visit between February 1, 1996, and January 30, 1999, to December 31, 2011. The data was analyzed from May 2015 to October 2015. The findings were replicated in an administrative cohort of 248 751 patients with an estimated glomerular filtration rate of at least 60 mL/min/1.73 m2 from the Geisinger Health System. An Error Occurred Setting Your User Cookie. This site uses cookies to improve performance.

If your browser does not accept cookies, you cannot view this site. Setting Your Browser to Accept Cookies There are many reasons why a cookie could not be set correctly. Below are the most common reasons: 00492520. Problem loading page. Soapware usersguide.pdf. OpenIn. OpenIn. 1-130221151440.pdf. Ki2015155a.pdf. Disease definitions linked to pharmaceutical companies. A few weeks ago, ABC Radio aired a frightening item stating one in 10 Australians has “chronic kidney disease”, CKD, and most don’t know they have it.

The story prominently featured fear of early death, and the salutary tale of a young man who belatedly discovered advanced kidney disease needing medical attention. What the ABC story didn’t reveal was that the definition of kidney disease has been dramatically and controversially expanded in recent years by experts and organisations with direct links to pharmaceutical companies.
Welcome to Forbes. America’s Epidemic of Unnecessary Care. It was lunchtime before my afternoon surgery clinic, which meant that I was at my desk, eating a ham-and-cheese sandwich and clicking through medical articles.

Among those which caught my eye: a British case report on the first 3-D-printed hip implanted in a human being, a Canadian analysis of the rising volume of emergency-room visits by children who have ingested magnets, and a Colorado study finding that the percentage of fatal motor-vehicle accidents involving marijuana had doubled since its commercial distribution became legal. The one that got me thinking, however, was a study of more than a million Medicare patients. It suggested that a huge proportion had received care that was simply a waste. The researchers called it “low-value care.” Update on Medical Overuse. CCDR: Volume 41 S-4, June 18, 2015. To share this page just click on the social network icon of your choice.

Canada Communicable Disease Report CCDR ISSN 1481-8531 (On-line) Public Opinions about Overdiagnosis: A National Community Survey. Abstract Background Despite evidence about the "modern epidemic" of overdiagnosis, and expanding disease definitions that medicalize more people, data are lacking on public views about these issues.
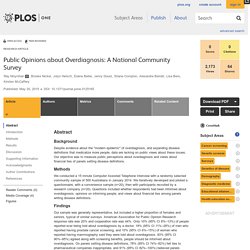
Our objective was to measure public perceptions about overdiagnosis and views about financial ties of panels setting disease definitions. Methods. Carlos Martins: Overuse of medical tests—a new health risk factor? A risk factor is, among other things, an aspect of personal behaviour or lifestyle that, on the basis of epidemiologic evidence, is known to be associated with health related conditions considered important to prevent (1).
A new behaviour may be observed in the general population of western countries; a behaviour related to the way patients use medical services with preventive intention and the frequency that they receive medical tests and other screenings. Evidence shows an alarming tendency to overuse preventive health services (2,3). In Portugal, for example, a recent population-based cross-sectional study showed that the majority of Portuguese adults think they should undergo general routine blood and urine tests on an annual basis.
Other, even less-recommended screening tests, such as lung X-rays, breast ultrasounds, abdominal ultrasounds, and gynaecological ultrasounds, are deemed necessary by a great proportion of the population (3). How risk factors drive medical overtreatment – Jeff Wheelwright. Most health-conscious people are familiar with the concept of risk factors for disease.
We’re too familiar, in fact. A risk factor is like the guest that nobody invited to the party, a spoiler. Though we might feel fine now, our individual risk for (fill in the blank) tells us that our wellbeing might not last. That vague and remote prospect of a stroke or a tumour has taken on a sharply numerical precision, thanks to screening tests that expose and quantify our risk factors. Less is More: The dangers of too much medicine - Students 4 Best Evidence. Posted on January 16, 2015 Tags: Cochrane, cost of care, Healthcare triage, JAMA, less is more, over-diagnosis, overtreatment Key message Many people throughout the world are rightly concerned that they are not getting enough of the quality healthcare they need.
Yet, there is also a growing concern that the opposite issue of overtreatment, and too much medicine, is actually causing harm, as well as increasing costs of care. 'Less Is More': The Next Big Thing for Medicine. When billionaire-entrepreneur-Dallas Mavericks owner Mark Cuban lobbed a Tweet in early April advising his followers to have their blood tested "for everything available" every 3 months, he probably didn't expect to unleash a Twitterspheric debate on medical overuse.
Scores of health journalists and clinicians jumped on this ill-advised tweet, explaining that such overtesting can result in false positives, further testing, unneeded treatment, patient stress, and considerable costs. Although it's unlikely that the furor swayed opinions on either side, it reflects a larger, thoughtful conversation within the healthcare community. That discussion is the "less is more" movement to reduce overuse of "low-value" services such as screening, diagnostic tests, or treatments that are unlikely to help patients and pose risk of harm.
Pro/Con: ‘Unnecessary’ Testing. By William Sullivan, DO, JD, Jerome Hoffman, MD, Hemal Kanzaria, MD, Marc Probst, MD & Judith Tintinalli, MD on June 29, 2015 Part of a series. Click here to read Night Shift: Throwing Stones. In March, the Journal of Academic Emergency Medicine published a study entitled ‘Emergency Physician Perceptions of Medically Unnecessary Advanced Diagnostic Imaging’. The study, authored by Kanzaria, Hoffman, Probst, Caloyeras, Berry & Brook, concluded that “many EPs believe a substantial proportion of [advanced imaging] studies, including some they personally order, are medically unnecessary.”
This garnered headlines in the lay press, as well as a blog post on EPM’s site, which prompted a response from Jerry Hoffman, one of the study authors. The Bow Tie Model of 21st Century Palliative Care. The Bow Tie Model of 21st Century Palliative Care The World Health Organization’s (WHO) definition of palliative care1 has evolved such that the recipient’s illness is no longer required to be deemed incurable. Palliative care is now described as an approach applying to “life-threatening illness”, and “applicable early in the course of illness, in conjunction with other therapies that are intended to prolong life”. This modern definition aims to include patients at a stage in their illness when cure may be unlikely, but not impossible. Disease definitions linked to pharmaceutical companies. Pointofcarejournals.