

One dead, four hospitalized after receiving OpenBiome stool transplants. Unlock this article — plus daily coverage and analysis of the biopharma sector — by subscribing to STAT Plus.
First 30 days free. What is it? STAT Plus is STAT's premium subscription service for in-depth biotech, pharma, policy, and life science coverage and analysis. Our award-winning team covers news on Wall Street, policy developments in Washington, early science breakthroughs and clinical trial results, and health care disruption in Silicon Valley and beyond. Long-Term Gut Microbial Changes After FMT – Lacto Bacto. Undergoing Microbiota Transplant Therapy. Cost-effectiveness analysis of fecal microbiota transplantation for inflammatory bowel disease. Inflammatory bowel disease (IBD), comprising ulcerative colitis (UC) and Crohn’s disease (CD), is a chronic disease characterized by a relapsing and remitting course [1].

Genetics, immunology, gut microbial dysbiosis and environmental factors were involved in the pathogenesis of IBD [1, 2]. The incidence of IBD is increasing in Asia, from the results of a territory-wide IBD registry in Hong Kong, the adjusted prevalence of IBD, UC, CD, and IBD unclassified per 100,000 individuals in 2014 were 44.0, 24.5, 18.6, and 0.9, respectively [3]. Medical management of IBD involves the acute treatment for the induction of remission, followed by the maintenance of remission. Everything You Wanted to Know About Fecal Transplants. The great fecal microbiota transplant debate — The American Microbiome Institute. An article was published today in the Atlantic that does a really nice job of describing the controversy surrounding fecal microbiota transplants (FMTs).
Basically, FMTs have been highly effective (>90% effective) in treating C. Difficile infections, and this efficacy has been even used as proof of the causal role of dysbiosis in C. Diff infection. The problem though, is that FMTs are currently unregulated, and the real question is how does the FDA regulate this new treatment, especially with how little is known about the microbiome. The first question the FDA has to answer is whether or not fecal microbiota is a drug or a tissue. RHR: Fecal Microbiota Transplants. In this follow-up interview with Glenn Taylor of the Taymount Clinic in the U.K., we discuss the latest developments in fecal microbiota transplant (FMT).
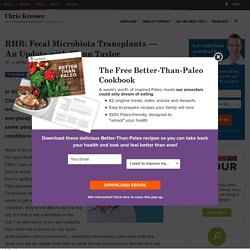
A Bitter Pill. By Arielle Duhaime-Ross | Photography by Vjeran Pavic Human feces floated in saline solution in a mortar, on a marbled countertop, in a dimly lit kitchen in Burlingame, California.

A bottle of ethyl alcohol, an electronic scale, test tubes, and a stack of well-worn pots and pans lay nearby. The stove light illuminated the area as Josiah Zayner crushed the shit with a pestle, creating a brownish-yellow sludge. "I think I can feel something hard in there," he said, laughing. It was probably vegetables — "the body doesn’t break them down all the way. " This heralded the beginning of Zayner’s bacterial makeover. Over the course of the next four days, Zayner would attempt to eradicate the trillions of microbes that lived on and inside his body — organisms that helped him digest food, produce vitamins and enzymes, and protected his body from other, more dangerous bacteria.
Zayner unwrapped a brand-new syringe and filled its barrel with the brownish liquid. Clostridium difficile Infection after Implementation of FMT In a recent issue of Annals of Internal Medicine, Cammarota et al. showed that the implementation of a fecal microbiota transplantation (FMT) program, available from June 2013 in the A.

Gemelli University Hospital, an Italian academic tertiary care centre, led to fewer surgical procedures for severe C. difficile infection (CDI). Between January 2010 and April 2015, 901 patients with CDI were identified, with a gradual increase over time (2010= 54 patients; 2011= 116 patients; 2012= 200 patients; 2013= 212 patients; 2014= 268 patients; January-April 2015= 71 patients). Thirty-five patients with severe cases underwent FMT: 7 in 2013, 16 in 2014, and 12 between January and April 2015. Faecal microbiota transplantation: a regulatory hurdle? In 2013, the first randomized controlled open-label clinical trial examining the therapeutic advantages of faecal microbiota transplantation versus vancomycin treatment was published by van Nood et al. [34]; they randomly assigned 43 patients (41 patients completed the study) with recurrent C. difficile infection to one of the 3 treatment regimens: (I) patients received a short vancomycin treatment (4–5 days of 500 mg 4 times/day), followed by a bowel lavage and faeces transplant via a nasoduodenal tube (17 patients with 1 patient excluded during the study), (II) vancomycin treatment (500 mg 4 times/day during 14 days) (13 patients with 1 patient excluded during the study), and (III) vancomycin treatment (500 mg 4 times/day during 14 days) with bowel lavage at day 4–5 of the treatment (13 patients).
After the first randomized controlled trial, as performed by van Nood et al. [34], additional randomized controlled studies have been published [36, 37, 38, 39, 40]. Cost-effectiveness analysis of fecal microbiota transplantation for inflammatory bowel disease. Sepsis-like syndrome in a patient after Fecal Microbiota Transplant — The American Microbiome Institute. Clostridium difficile infection causes pain and diarrhea, is sometimes fatal, and normally occurs after a course of antibiotics leaves the gut in a state of dysbiosis where the C. diff can thrive.

Doctors normally prescribe antibiotics to cure this infection, but this can sometimes exacerbate the problem, making the gut even more prone to infection. Fecal microbiota transplants (FMT) are the most successful therapy to treat the condition and have been seen to be successful in as many as 95% of treatments. A group of doctors in California chronicled the story of a 56-year-old woman who suffered from C. diff after she took a 10-day course of amoxicillin after she became sick with bacterial sinusitis. She went to the doctor after getting very sick and reporting 8-10 bowel movements per day. She was then prescribed various other antibiotic regimes that did not improve her condition over several days and a stool analysis found that she had C. diff.
Treating C. difficile without antibiotics — The American Microbiome Institute. I recently had the pleasure of hearing a talk by Professor Xinhua Chen from the Beth Israel Deaconess Medical Center about various ways to treat C. difficile infections without antibiotics.

As we know, antibiotics are often successful in treating C. diff infections. However, 30% of all treated infections result in a relapse, likely due to the fact that these antibiotics kill commensal bacteria which are needed to keep C. diff populations low. In addition, Dr. Chen discussed how other bacteria can act as a 'sink' for the C. diff. toxins, which, when they bind to other bacteria, do not harm humans. Therefore Dr. Host inflammatory response is often the danger in C. Insight into microbiota transplants. In spite of being a technique that professionals began to practice and research decades ago, gut microbiota transplantation is an issue that is sparking considerable interest right now as a possible treatment for infections of the intestine (especially those produced by the Clostridium difficile bacteria).

Professor Lawrence Brandt, of the Albert Einstein College of Medicine (USA), is one of the pioneers of this method. We interviewed him during the 2nd Gut Microbiota and Health Summit and he explained what the treatment (also called ‘faecal transplantation’) involves, when and how it is carried out and the scientific evidence available regarding this technique – an issue that generates both debate within the scientific community and interest in the media. Mark Smith of OpenBiome: Should Scientists Supervise Patients Who Self-Administer FMTs. Dr. Mark Smith is a postdoctoral associate at Massachusetts Institute of Technology and co-founder of OpenBiome, a nonprofit organization focused on expanding safe access to fecal microbiota transplantation (FMT).
Smith attended the Fourth Gut Summit in Barcelona on March 14th and 15th, 2015. (See replays of the event here.) After the summit, he answered some questions for GMFH editors about a recent provocative opinion piece on FMT. Dr. How much variation do you see in the way FMT is administered in different places? There is considerable variation in the mode of delivery for FMT.
Science or pretense? FMTs for conditions other than C. difficile? Fecal microbiota transplantation (FMT), which is up to 90% effective in treating recurrent Clostridium difficile (C. difficile) infection, may or may not be an effective treatment for other conditions. Researchers around the world are investigating its use for ulcerative colitis, Crohn’s disease, and more. Regulatory bodies have not approved its use for conditions other than C. difficile, but that doesn’t stop thousands of people from trying FMT at home. An estimated 10,000 people per year are doing FMT without permission and without supervision, according to Catherine Duff, founder and president of patient advocacy organization The Fecal Transplant Foundation. Journalist David Wild recently spoke with Duff and reported that individuals are self-administering FMT for conditions as diverse as Crohn’s disease and ulcerative colitis, autism, depression, diabetes, and multiple sclerosis.
Jessica Richman, co-founder of uBiome, agrees that the problem needs to be addressed with more studies. Faecal microbiota transplantation for Gastrointestinal Diseases. Stool transplants highly efficient for Clostridium difficile infections and other gastrointestinal conditions — online press conference at 2nd World Summit “Gut Microbiota For Health” held today (26 February 2013) Clostridium difficile infections have developed into a virtual pandemic over the past two decades. The outcome of standard antibiotic treatment is unsatisfactory: the recurrence rates are high with every relapse increasing the risk of further follow-ups. Fecal microbiota transplant as a treatment for MRSA enterocolitis — The American Microbiome Institute.
Fecal microbiota transplants (FMTs) are most commonly used for treating Clostridium difficile infection, an often lethal bacterial infection of the gut. However, there have been many hypotheses that FMTs could be used to treat other conditions that result in a dysbiosis of the microbiota. A new study published in BMC Infectious Diseases suggests that FMTs could be used to treat enterocolitis, infection of the gut, that is a result of Methicillin-resistant Staphylococcus aureus (MRSA).
The most common treatment for this to date has been antibiotic treatment, specifically vanomycin, but the results of how this impacted the microbiota were not measured. New info on fecal microbiota transplants for C. difficile and ulcerative colitis — The American Microbiome Institute. Two important papers regarding fecal microbiota transplants (FMTs) were published last week.
The first was an examination of a patient’s microbiome over time after he or she undergoes an FMT to treat C. difficile. The second showed the results of clinical trials that used FMTs in an attempt to treat ulcerative colitis. The FMT papers, which are described below, improve our understanding of this procedure, which holds promise to treat various microbiome-based diseases. The C. diff paper, published in the journal Microbiome, attempted to answer the question: Do the microbiome changes that occur after FMT remain long after the procedure? Fecal microbiota transplant as a potential therapy for Crohn's disease — The American Microbiome Institute. Refractory Crohn's disease with fecal microbiota transplantation. Dr. Faming Zhang, MD, PhD, is a doctor and researcher at the Institute for Digestive Endoscopy & Medical Center for Digestive Diseases at The Second Affiliated Hospital of Nanjing Medical University in Nanjing, China. He is Vice Chief of the Medical Center for Digestive Diseases, and Director of Intestinal Diseases.
Fecal microbiota transplants for pouchitis not yet effective — The American Microbiome Institute. Should we exclude obese donors from FMT? Neha Alang and Colleen R. Transfer of Viral Communities between Human Individuals during Fecal Microbiota Transplantation. Fecal Transplant Pill Fails Trial. What Diane Hoffman said is insightfully correct and should be engraved into researchers' minds: “I have this theory that there’s something potentially unique about the composition of microorganisms together that produces the beneficial effect. Fecal Microbiota Transplants: Current Knowledge and Future Directions. Transplanted Fecal Microbes Stick Around. Antibiotic treatment eliminates many commensal bacterial species from the gut lumen, but fecal transplants can restore a healthy microbial community.SCIENCE, E.
Tracking Fecal Transplants.