

Amy Curzon
Future Healthcare in Canada Focus Indigenous Populations. Vulnerable Populations. Chronic disease. Mock Code Scenarios. Spheres of Influence on Health. What is Health. Determinants of Health. Indigenous Health. Health Promotion. Federal and Provincial Health Systems in Canada. Public Health Agency of Canada.
Ministry of Health and Long-Term Care. Single-Payer - Good, Bad, and Ugly of the Canadian System — JournalFeed. Written by Clay Smith Why talk about this?
Universal healthcare coverage is a hot topic but one that many of us know surprisingly little about, beyond surface level slogans from campaign signs or bumper stickers. I'm hoping to learn more with this JAMA Internal Medicine article about the Canadian single-payer system. What little I know about Canadian healthcare comes from this article. I am summarizing what these authors have written and make it clear when I am speaking my own opinion. Healthcare Financing - Canadian Style Satisfaction over TimeThere was initial patient enthusiasm for the single-payer model begun in Canada. The GoodEvery Canadian with legal status has healthcare covered. The BadHospital closures and physician income caps have led to some physicians leaving, an increase in wait times, and decrease in access for some patients. The UglyIt is unlikely the system will change.
My Thoughts I now leave the confines of the JAMA Internal Medicine article. Finger on the pulse? Sources. Understand how health care works in Canada. If you are a Canadian citizen or permanent resident, you may apply for public health insurance.
With it, you don’t have to pay for most health-care services. The universal health-care system is paid for through taxes. When you use public health-care services, you must show your health insurance card to the hospital or medical clinic. Each province and territory has their own health insurance plan. Make sure you know what your plan covers. All provinces and territories will provide free emergency medical services, even if you don’t have a government health card. If you have an emergency, go to the nearest hospital. In some provinces you must wait, sometimes up to three months, before you can get government health insurance.
You need a health insurance card from the province or territory where you live to get health care in Canada. 's Health Care System. Table of Contents Introduction Canada's publicly funded health care system is dynamic--reforms have been made over the past four decades and will continue in response to changes within medicine and throughout society.

The basics, however, remain the same--universal coverage for medically necessary health care services provided on the basis of need, rather than the ability to pay. Background The basic values of fairness and equity that are demonstrated by the willingness of Canadians to share resources and responsibility are displayed in Canada's health care system, and have been reflected in the modifications and major reforms made to the system since its inception. Evolution of Our Health Care System In general, Canada's Constitution sets out the powers of the federal and the provincial and territorial governments. Before World War II, health care in Canada was, for the most part, privately delivered and funded. In 1984, federal legislation, the Canada Health Act, was passed. AHA Telemetry Guidelines Improve Telemetry Utilization in the Inpatient Setting.
Study Design: We used Plan-Do-Study-Act cycles with chart review for pre- and postintervention measurement collection.
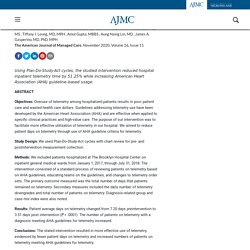
Methods: We included patients hospitalized at The Brooklyn Hospital Center on inpatient general medical wards from January 1, 2017, through July 31, 2018. The intervention consisted of a standard process of reviewing patients on telemetry based on AHA guidelines, educating teams on the guidelines, and changes to telemetry order sets. The primary outcome measured was the total number of days that patients remained on telemetry. Secondary measures included the daily number of telemetry downgrades and total number of patients on telemetry. Diagnosis-related group and case mix index were also noted. Results: Patient average days on telemetry changed from 7.20 days preintervention to 3.51 days post intervention (P < .0001).
Am J Manag Care. 2020;26(11):476-481. Takeaway Points The study period was 18 months, from January 1, 2017, through July 31, 2018.