

Effects of Beta-Hydroxy-Beta-Methylbutyrate Supplementation on Elderly Body Composition and Muscle Strength: A Review of Clinical Trials - FullText - Annals of Nutrition and Metabolism. Costa Riela N.A.a · Alvim Guimarães M.M.a · Oliveira de Almeida D.b,c · Araujo E.M.Q.b,d Author affiliations aLife Sciences Department, University of The State of Bahia (UNEB), Bahia, BrazilbLife Sciences Department, Nucleus of Research and Extension in Nutritional Genomics and Metabolic Dysfunctions (GENUT), University of The State of Bahia (UNEB), Salvador, BrazilcProfessor of undergraduate medical course, UniFTC, Salvador, BrazildLife Sciences Department/UNEB, Health Sciences Institute/UFBA, Coordinator of Nutrition Course and GENUT, Professor at Post-Graduation Program Interactive Process of Organs and Systems, Salvador, Brazil Contact Author Edilene Maria Queiroz Araujo.

Nutritional Management Enhances the Recovery of Swallowing Ability in Older Patients with Sarcopenic Dysphagia. This study assessed whether a high provided energy of ≥30 kcal/ideal body weight (IBW)/day (kg) for patients with sarcopenic dysphagia effectively improved swallowing ability and the activities of daily living (ADLs).

Among 110 patients with sarcopenic dysphagia (mean age, 84.9 ± 7.4 years) who were admitted to a post-acute hospital, swallowing ability and the ADLs were assessed using the Food Intake LEVEL Scale (FILS) and the Functional Independence Measure (FIM), respectively. The primary outcome was the FILS at discharge, while the secondary outcome was the achievement of the FIM with a minimal clinically important difference (MCID) at discharge. Dysphagia in Older Adults - Mayo Clinic Proceedings. Nutrients to mitigate osteosarcopenia: the role of protein,... AGEING: BIOLOGY AND NUTRITION: Edited by Jürgen M.
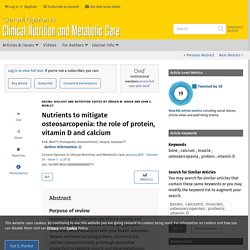
Bauer and John E. Morley. Protein Intake and Frailty: A Matter of Quantity, Quality, and Timing. Frailty is a geriatric syndrome that refers to a state of reduced resiliency to stressful events that occurs in response to physiological and/or psychosocial detriments.
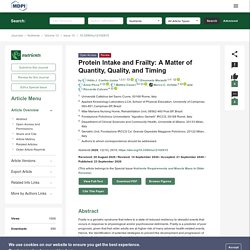
Frailty is a predictor of poor prognosis, given that frail older adults are at higher risk of many adverse health-related events. Hence, the identification of potential strategies to prevent the development and progression of frailty is of extreme importance for avoiding its negative outcomes. An adequate protein consumption is advocated as a possible intervention for the management of frailty in older adults due to its effects on muscle mass and physical function. However, empirical evidence is still needed to support this proposition. On the other hand, substantial evidence from observational studies has provided important information on the association between frailty and dietary protein-related parameters. ►▼ Show Figures Figure 1. Nutrition Mediates the Relationship between Osteosarcopenia and Frailty: A Pathway Analysis.
Osteosarcopenia is associated with increased risk of adverse outcomes such as falls and fractures.

Its association with frailty is less well-described, particularly in independent community-dwelling older adults. Although nutrition plays a crucial role in maintaining bone and muscle health, the complex relationship between osteosarcopenia and nutrition in the pathogenesis of frailty remains to be elucidated. In this cross-sectional analysis of 230 independent, community-dwelling individuals (mean age 67.2 ± 7.4 years), we examined the associations between osteosarcopenia with nutritional status and frailty, and the mediating role of nutrition in the association between osteosarcopenia and frailty. ►▼ Show Figures.
A clinical guide to the pathophysiology, diagnosis and treatment of osteosarcopenia - Maturitas. Reginster J.Y.
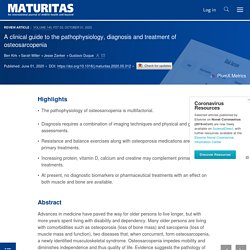
Beaudart C. Buckinx F. Bruyère O. Should the Energy Contribution of Commercial Thickeners Be Considered in the Nutrition Plan of Patients With Dysphagia? - Miranda - 2020 - Nutrition in Clinical Practice. Background: Clinical management options for dysphagia include the use of thickeners to increase the consistency of liquids.
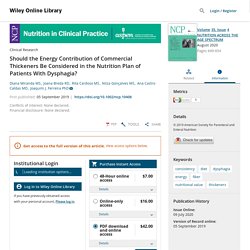
Health professionals may not be aware of the nutrition value of these products, since there are no such recommendation in clinical guidelines. Our aim was to estimate the added nutrition value of the 2 types of commercial thickeners (starch and xanthan gum) to daily nutrition intake and compare their nutrition value for nectar, honey, and pudding consistencies. Additionally, we compared the nutrition value of both thickeners with a high‐energy powder, since they share the same main ingredients. Methods: We collected recommended dosages for obtaining the 3 different consistencies and nutrition content from the technical food labels.
Nutrition and Sarcopenia—What Do We Know? Sarcopenia consists of a loss of skeletal muscle mass and physical function (muscle strength or physical performance) that occurs with advancing age and has become increasingly prevalent [1,2,3].
Sarcopenia causes concern because it may result in many adverse outcomes for older adults, including physical disability, poor quality of life, and increased mortality [2]. Sarcopenia is responsible for considerable healthcare expenditure, with direct medical costs attributable to the disorder estimated at US $18.5 billion in the United States in 2000 [4]. Sarcopenia generally refers to class II sarcopenia, which is defined as individuals with an appendicular skeletal muscle mass (ASM)/height^2 ratio below 2 SD. Texture-Modified Diet for Improving the Management of Oropharyngeal Dysphagia in Nursing Home Residents: An Expert Review. The context of the NH The long-stay NH resident population has specific characteristics marked by a shorter life expectancy relative to community-dwelling older adults, high prevalence of multimorbidity with a high rate of complications, dementia, frailty, disability, and often polypharmacy.

Oropharyngeal dysphagia (OD), defined as the inability to initiate and perform safe swallowing (1, 2), alongside poor coordination and propulsion, may result in aspiration from the passing of food, a liquid bolus, or regurgitated gastric contents into the respiratory tract, and is believed to be common among this population (3). This population also has a significantly greater risk of malnutrition, resulting from a variety of challenges including the oral processing of food (4).
Due to the large heterogeneity within the NH resident population, defined resident-specific care needs, including nutritional goals, are urgently required. התאמת מרקמי מזון ושתייה עבור אנשים עם הפרעת בליעה. Lack of Standardization in Commercial Thickeners Used in the Management of Dysphagia - Abstract - Annals of Nutrition and Metabolism 2019, Vol. 75, No. 4. Ann Nutr Metab 2019;75:246–251 To view the fulltext, please log in To view the pdf, please log in Buy FullText & PDF Unlimited re-access via MyKarger Unrestricted printing, no saving restrictions for personal use read more Select.

Post-extubation dysphagia: a problem needing multidisciplinary efforts. Sarcopenia: A Time for Action. An SCWD Position Paper - Bauer - - Journal of Cachexia, Sarcopenia and Muscle. Physical Frailty: ICFSR International Clinical Practice Guidelines for Identification and Management. These guidelines were formed by the International Conference of Frailty and Sarcopenia Research (ICFSR) which is an international alliance of subject-matter experts in the fields of both frailty and sarcopenia. An ICFSR expert working group on frailty (referred to as the ‘task force’ hereon) was formed, and included a multidisciplinary panel of practicing clinicians (predominantly geriatricians), Allied Health Professionals (AHPs), Primary Care Physicians (PCPs), musculoskeletal physiologists, gerontologists, and methodology experts.
A steering committee was formed from the task force members, and was responsible for overseeing the development and review of the guideline development process. Management of Malnutrition in Older Patients—Current Approaches, Evidence and Open Questions. 3.1. Lacking Evidence in Many Fields Despite increasing numbers of systematic reviews on the topic, more than half of the recommendations in the ESPEN guideline are “good practice points”, meaning that they are based on the clinical experience of the guideline development group because of a lack of studies [49]. Nutritional interventions to prevent and treat frailty : Current Opinion in Clinical Nutrition & Metabolic Care. Dietary Factors Associated with Frailty in Old Adults: A Review of Nutritional Interventions to Prevent Frailty Development. 4.2.1. Proteins Although the ‘ideal’ diet for elderly people is not yet known, it seems clear that it is necessary to maintain muscle mass.
Basically, there are two ways to do this: On the one hand, an individual can build new muscle mass, and on the other hand, an individual can stop the decrease of muscle. Evidently, the latter seems to be more interesting for the elderly population, specifically for frailty subjects. Although numerous clinical trials have been carried out to evaluate the effect of protein supplementation on muscle mass, in the present review, we focus solely on those trials performed to avoid the development or treatment of frailty syndrome, which are summarised in Table 1. Table 1. The first trial to this end was conducted in 2013 by Kim and Lee. In 2016, Porter Starr et al. performed a similar work on obese older adults with low physical performance [45].
A similar study was also performed by Collins et al. [46]. 4.2.2. 4.2.3. 4.2.4. Table 2. Malnutrition Screening and Assessment in Hospitalised Older People: A Review. Adopt the IDDSI for Dysphagia – RDLounge.com. Marsha is an RD and clinical nutrition coordinator for a small chain of skilled nursing facilities. When attending the Academy of Nutrition and Dietetics (Academy) Food & Nutrition Conference & Expo™ in October 2018, she learned that the Academy and the American Speech-Language Hearing Association both support the International Dysphagia Diet Standardisation Initiative (IDDSI).
On the heels of the Academy’s May 1, 2019, IDDSI implementation date, Marsha realized that now is the time for both RDs and speech-language pathologists to take the leap and become comfortable with the framework, food and fluid consistencies, new terminology, and testing methods for dysphagia. At her suggestion, her company decided to implement the IDDSI in every facility. Marsha is preparing for an upcoming meeting for corporate management staff and facility management staff to introduce IDDSI and discuss a plan to adopt it companywide.
Where Should Marsha Begin? Like this: Like Loading... Optimal Protein Intake during Weight Loss Interventions in Older Adults with Obesity: Journal of Nutrition in Gerontology and Geriatrics: Vol 38, No 1. Treatment of obesity in older persons—A systematic review - Haywood - 2019 - Obesity Reviews. Anorexia of Aging - An Updated Short Review. Things We Do for No Reason: The Use of Thickened Liquids in Treating Hospitalized Adult Patients with Dysphagia. Inspired by the ABIM Foundation's Choosing Wisely campaign, the “Things We Do for No Reason” (TWDFNR) series reviews practices that have become common parts of hospital care but may provide little value to our patients. Practices reviewed in the TWDFNR series do not represent “black and white” conclusions or clinical practice standards but are meant as a starting place for research and active discussions among hospitalists and patients.
We invite you to be part of that discussion. A 74-year-old man with Alzheimer’s dementia and chronic dysphagia with a history of aspiration pneumonia presents with urinary tract infection, hypovolemia, and hypernatremia. He has been on thickened liquids at home for the past several months. As his overall condition improves with intravenous fluids and antibiotics, he requests to drink thin liquids. Dysphagia is defined as difficulty or discomfort with feeding or swallowing1 and is a common clinical problem facing hospitalists. Disclosures. Dysphagia: Interprofessional Management, Impact, and Patient‐Centered Care - McGinnis - 2019 - Nutrition in Clinical Practice. Introduction. Rehabilitation Nutrition for Iatrogenic Sarcopenia and Sarcopenic Dysphagia. Sarcopenia and dysphagia: Position paper by four professional organizations - Fujishima - 2019 - Geriatrics & Gerontology International. International Clinical Practice Guidelines for Sarcopenia (ICFSR): Screening, Diagnosis and Management.
Does nutrition play a role in the prevention and management of sarcopenia? - Clinical Nutrition. Recent advances in pharmacological, hormonal, and nutritional intervention for sarcopenia. Best practice guidelines for the management of frailty: a British Geriatrics Society, Age UK and Royal College of General Practitioners report. + Author Affiliations Address correspondence to: G.
Turner, Tel (+44)2076081369; Fax (+44)2076081041, Email: quality@bgs.org.uk. Received June 24, 2014. Accepted July 8, 2014. Abstract Older people are majority users of health and social care services in the UK and internationally. The British Geriatrics Society Fit for Frailty guideline is consensus best practice guidance for the management of frailty in community and outpatient settings.
Protein intake and exercise for optimal muscle function with aging: Recommendations from the ESPEN Expert Group. Frailty Consensus: A Call to Action. To view the full text, please login as a subscribed user or purchase a subscription. Click here to view the full text on ScienceDirect. Fig. 1 Clinical Frailty Scale. Scoring is based on clinical judgment.
Abstract Frailty is a clinical state in which there is an increase in an individual’s vulnerability for developing increased dependency and/or mortality when exposed to a stressor. 1.Physical frailty is an important medical syndrome.