

Accurate vital sign monitoring serves as the foundational skill for every medical professional enterin the clinical field.
The aneroid sphygmomanometer from MedTechKits provides the essential tactile feedback and mechanical reliability required to master this critical diagnostic technique.
Developing a deep understanding of manual pressure measurement ensures that a practitioner can operate effectively when electronic systems fail.
Every specific part of the instrument plays a definitive role in capturing precise physiological data during a patient assessment.
Familiarizing oneself with the structural design is the first step toward achieving the clinical excellence detailed in this professional guide.
MedTechKits focuses on equipping first responders with caliberated tools that connect classroom theory with EMS application.
Each specialized medkit is curated to ensure that EMTs and paramedics have immediate access to dependable instruments that perform under the most rigorous field conditions.
By prioritizing durability and precision, the organization supports the professional growth of medical students throughout their clinical rotations.
This commitment to quality ensures that every practitioner feels prepared to deliver life-saving care with total confidence in their equipment.
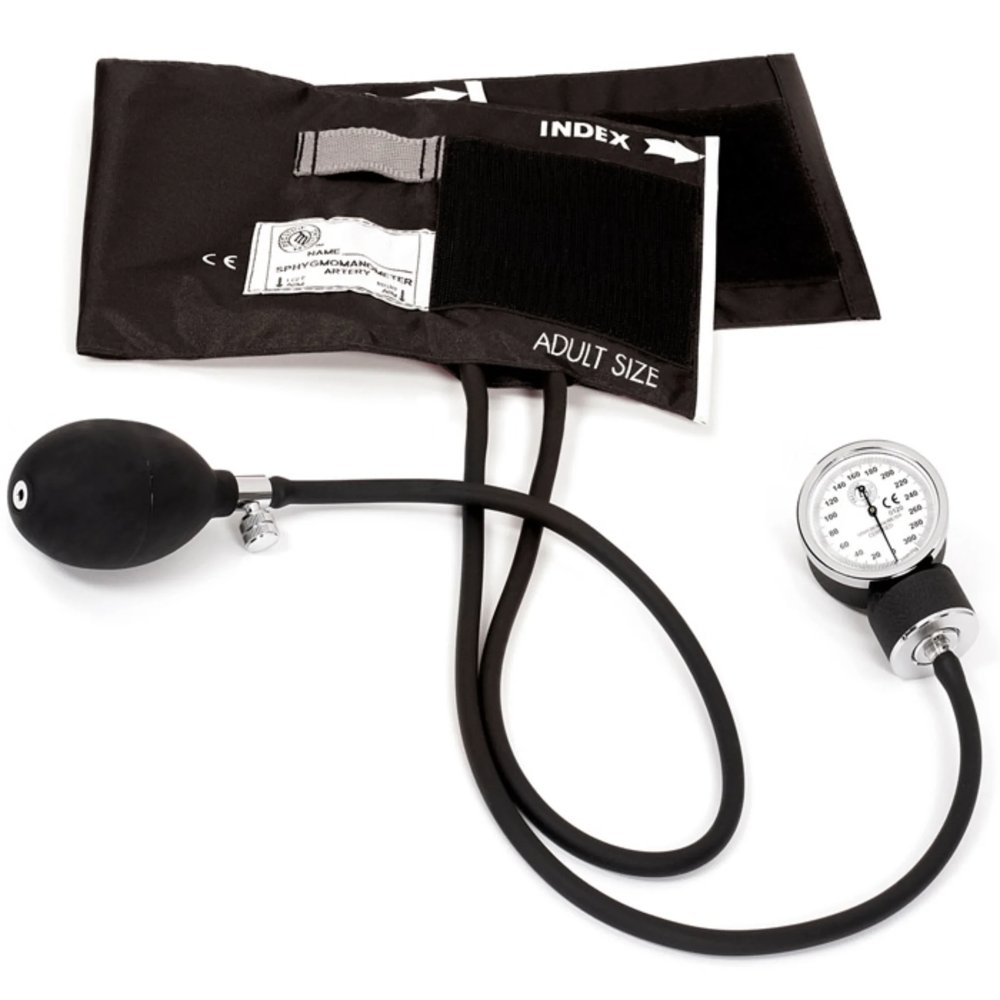
The aneroid sphygmomanometer from MedTechKits remains an indispensable instrument for clinicians who require immediate and accurate hemodynamic data.
Its design emphasizes a tactile connection between the practitioner and the patient, ensuring a high level of clinical engagement during every assessment.
Understanding the mechanical nature of this tool is the first step toward mastering manual blood pressure measurement.
The device is engineered to withstand the environment of emergency medical services while maintaining its calibration over time.
The core of the system consists of several integrated parts that work in harmony to occlude and release blood flow.
A high-quality inflation bulb allows the user to build pressure within the bladder, while the manometer provides a visual representation of that pressure in millimeters of mercury.
Beyond the internal mechanics, the exterior elements are designed for both patient comfort and user efficiency.
The connection tubing is built to resist kinking, ensuring that the airflow remains consistent and the gauge reacts instantly to pressure changes.
The cuff is constructed from a durable, latex-free nylon material that prioritizes both hygiene and longevity in a clinical setting.
It features specialized index and range markings that guide the clinician in selecting the correct size for the patient's arm circumference.
In addition to size markings, the cuff includes a dedicated artery indicator to ensure precise alignment over the brachial artery.
This placement is essential for capturing the most accurate Korotkoff sounds during the auscultation process.
The precision manometer features a large, high-contrast dial that allows for easy reading even in low-light emergency environments.
In a comprehensive training environment, students may use these manual tools alongside a lifepak simulator to learn how to cross-reference manual blood pressure readings with digital cardiac data.
Controlled deflation is managed by the knurled air release valve, which provides the tactile feedback necessary for a steady pressure drop.
By slowly rotating this valve, the practitioner can achieve the recommended deflation rate of two to three millimeters of mercury per second.
Manual sphygmomanometers are frequently cited as the gold standard because they are not susceptible to the electronic interference that can affect digital monitors.
While many people entering the healthcare field often ask how long does it take to become an emt, learning the art of manual auscultation is one of the most vital skills mastered during that training period.
They allow the clinician to listen directly to the physiological sounds of blood flow, providing a more nuanced understanding of the patient's cardiovascular state.
Clinicians often prefer the manual approach because it permits the detection of arrhythmias or faint pulses that automated machines might miss.
The process begins by securing the cuff snugly around the patient's upper arm and palpating the pulse to determine the initial inflation level.
The clinician then inflates the cuff rapidly before using the release valve to listen for the first rhythmic tapping sounds.
As the pressure continues to drop, the sounds eventually disappear, signifying the diastolic pressure or the heart at rest.
Recording these two distinct points provides a clear snapshot of the patient’s current circulatory health.
To ensure continued accuracy, the manometer should be regularly checked to confirm that the needle rests within the zero mark when the cuff is fully deflated.
The nylon cuff and inflation bulb should be wiped down with appropriate clinical disinfectants to prevent cross-contamination between patients.
Proper storage also plays a significant role in preserving the calibration of the internal bellows system.
Keeping the device in a protected case prevents the gauge from sustaining impact damage that could lead to inaccurate readings.
The adult aneroid sphygmomanometer proves its worth through its exceptional durability and its ability to function without a power source.
It offers a level of professional autonomy that allows clinicians to perform their duties with confidence in any situation.
Ultimately, the value of this instrument lies in its simplicity and the high degree of accuracy it provides to the trained user.
It serves as a testament to the fact that well-engineered mechanical tools are often the most dependable assets in healthcare.
Q1. How can I verify if my aneroid gauge is still properly calibrated before a shift?
Check the face of the gauge while the cuff is fully deflated; the needle must rest squarely within the small zero box at the bottom of the dial. If the needle sits outside this boundary, the internal mechanism may be out of alignment and requires professional recalibration to ensure patient safety.
Q2. What is the best way to clean the cuff after it has been exposed to fluids in the field?
The latex-free nylon material is designed for easy decontamination using standard quaternary ammonium or bleach-based clinical wipes. For a deeper clean, the bladder can be removed so the outer nylon sleeve can be hand-washed and air-dried to prevent cross-contamination.
Q3. Will this sphygmomanometer work accurately if it gets wet during an outdoor call?
The device is built to be water-resistant, but moisture trapped inside the manometer or the inflation bulb can interfere with the mechanical movement and lead to corrosion. If the unit is exposed to heavy rain, wipe it down immediately and ensure it is completely dry before storing it in its carrying case.
Q4. Does the gauge holder on the cuff accommodate left-handed users?
The integrated clip is designed to be versatile, allowing the manometer to be slid onto the cuff at various angles to suit the clinician's preference. This ensures that the dial remains clearly visible whether you are standing on the left or right side of the patient during a busy assessment.
1. Waterproof Notepad for EMS: Improve Accuracy in Patient Records
2. Smart Gear Management for EMTs Using the MedTech Backpack