

Medicare and Ambulance Svcs. Medicare Coverage of Ambulance Services. When does Medicare cover ambulance trips? Ambulance Services Center. Medicare vs. Medicaid. Medicare Interactive. Medicare.gov – the Official U.S. Government Site for Medicare. Coverage choice Original Medicare or a Medicare Advantage Plan. Part D is prescription drug coverage insurance that is provided by private companies approved by Medicare.
Diabetes Supplies. Medicare PDP Guide. How Self-Administered Drugs are handled. Plan Finder for Health, Prescription Drug and Medigap plans.
Check Your Enrollment. Part C is Medicare Advantange. Special Needs Plans - SNPs 11302. Preferred Provider Org's - PPOs 11152. Private Fee-for-Service - PFFS 10144. Part B is medical insurance. Diabetes Supplies. Medicare Premiums: Rules For Higher-Income Beneficiaries. If you have higher income, the law requires an adjustment to your monthly Medicare Part B (medical insurance) and Medicare prescription drug coverage premiums.
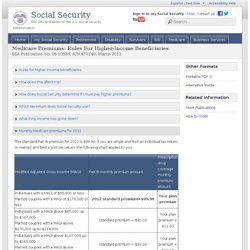
Higher-income beneficiaries pay higher premiums for Part B and prescription drug coverage. This affects . If you have higher income, you will pay an additional premium amount for Medicare Part B and Medicare prescription drug coverage. We call the additional amount the income-related monthly adjustment amount. Here’s how it works: Part B helps pay for your doctors’ services and outpatient care. If you are a higher-income beneficiary, you will pay a larger percentage of the total cost of Part B based on the income you report to the Internal Revenue Service (IRS). 11579.pdf (application/pdf Object) 2011 Part B Premium Amounts for Persons with Higher Income Levels. 2012 Part B Premium Amounts for Persons with Higher Income Levels.
Choosing MediGap (aka Medicare Supplement) Medigap Policy Search Home. View All Medigap Policies. Part A is hospital insurance. Choosing MediGap (aka Medicare Supplement) Medigap Policy Search Home. View All Medigap Policies. Medicare Booklet 2012. Your Medicare Benefits. Medicare Coverage of Diabetic Supplies & Services. Mental Health Benefits.
Getting Paid: Understanding Medicare's Mental Health Treatment Limitation - Nov-Dec 2000. Getting Paid Medicare significantly limits its mental health coverage, but you can protect your bottom line by knowing the rules.
Kent J. Moore Fam Pract Manag. 2000 Nov-Dec;7(10):15-16. Unfortunately, when you provide mental health services to your Medicare patients, your usual Medicare payments are reduced. What is the limitation? By law, Medicare payment for outpatient mental health services is limited to 62.5 percent of covered expenses incurred in any calendar year in connection with the treatment of a mental, psychoneurotic or personality disorder for an individual who is not an inpatient of a hospital at the time the expenses are incurred. What does it include? Three key components of the definition determine the scope of the limitation: “Treatment.” What isn't included? While Medicare's outpatient mental health treatment limitation can seem pretty broad, there are services that fall outside its scope, including the following: How is the limit applied?
Medicare Boosting Coverage For Mental Health Issues : Shots - Health News. Medicare coverage for people with depression used to be, well, depressing. But that's starting to change. In October, the Centers for Medicare and Medicaid Services began covering screening for depression without any cost-sharing when Medicare beneficiaries visit their primary care doctor. That's a big deal, because although older people have lower rates of depression than the general population — 10.7 percent, compared with 16.9 percent overall — they often have other chronic conditions that may worsen if their depression isn't treated.
And depression often goes undiagnosed in the elderly, who may feel the stigma of mental illness more acutely than younger people and are often less likely to seek help. Paying doctors to screen for depression — Medicare's going rate is $17.36 per person — might well increase how often they do it, experts say. "Doctors are trying to do the right thing, but how do you prioritize what to do in 21 minutes with a complex person? " Premiums and coinsurance rates for 2012.