

Clinical trial raises hope for cancer treatment - latimes.com. A microscopic image shows two T cells binding to beads, depicted in yellow,… (Dr.
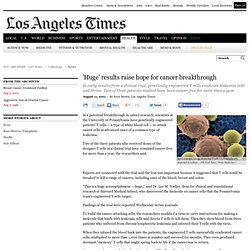
Carl June / Penn Medicine ) In a potential breakthrough in cancer research, scientists at the University of Pennsylvania have genetically engineered patients' T cells — a type of white blood cell — to attack cancer cells in advanced cases of a common type of leukemia. Two of the three patients who received doses of the designer T cells in a clinical trial have remained cancer-free for more than a year, the researchers said. Experts not connected with the trial said the feat was important because it suggested that T cells could be tweaked to kill a range of cancers, including ones of the blood, breast and colon. "This is a huge accomplishment — huge," said Dr. Findings of the trial were reported Wednesday in two journals. Penn Medicine News: Genetically Modified "Serial Killer" T Cells Obliterate Tumors in Patients with Chronic Lymphocytic Leukemia, Penn Researchers Report.
(PHILADELPHIA) -- In a cancer treatment breakthrough 20 years in the making, researchers from the University of Pennsylvania's Abramson Cancer Center and Perelman School of Medicine have shown sustained remissions of up to a year among a small group of advanced chronic lymphocytic leukemia (CLL) patients treated with genetically engineered versions of their own T cells.

The protocol, which involves removing patients' cells and modifying them in Penn's vaccine production facility, then infusing the new cells back into the patient's body following chemotherapy, provides a tumor-attack roadmap for the treatment of other cancers including those of the lung and ovaries and myeloma and melanoma. The findings, published simultaneously today in the New England Journal of Medicine and Science Translational Medicine, are the first demonstration of the use of gene transfer therapy to create "serial killer" T cells aimed at cancerous tumors.
Renewed hope for a cancer breakthrough with killer T cells - GlobalPost. Please support our site by enabling javascript to view ads.

Hope exists for a cancer breakthrough after scientists altered the T cells of leukemia sufferers — part of their own immune system — to successfully kill off cancer cells. Two of three patients who had the genetically modified T cells infused back into their body following chemotherapy, remained cancer-free for more than a year. One patient showed significant improvement. "This is a huge accomplishment — huge," Dr. Lee M. The treatment, pioneered by researchers at the University of Pennsylvania, involves infecting the white blood cells of patients with advanced chronic lymphocytic leukemia with a virus, and instructing those T cells to bind to cancer cells and ultimately kill them.
In each of the three patients studied, each virus-infected T cell killed about 1,000 cancer cells, according to the scientists' findings, published in the New England Journal of Medicine and Science Translational Medicine. Dr. T Cells with Chimeric Antigen Receptors Have Potent Antitumor Effects and Can Establish Memory in Patients with Advanced Leukemia. + Author Affiliations ↵†To whom correspondence should be addressed.
E-mail: cjune@exchange.upenn.edu AbstractBack to Top Tumor immunotherapy with T lymphocytes, which can recognize and destroy malignant cells, has been limited by the ability to isolate and expand T cells restricted to tumor-associated antigens. Chimeric antigen receptors (CARs) composed of antibody binding domains connected to domains that activate T cells could overcome tolerance by allowing T cells to respond to cell surface antigens; however, to date, lymphocytes engineered to express CARs have demonstrated minimal in vivo expansion and antitumor effects in clinical trials.
IntroductionBack to Top Using gene transfer technologies, T cells can be genetically modified to stably express antibody binding domains on their surface that confer novel antigen specificities that are major histocompatibility complex (MHC)–independent. CAR-mediated T cell responses may be further enhanced with addition of costimulatory domains.
Huge breakthrough in Cancer treatment using modified T-cells. Researchers at the University of Pennsylvania have genetically engineered patients’ T-cells to attack cancer cells in advanced cases of leukemia.

Two of three patients in the clinical trial have remained cancer free for a year. This is so fascinating to me. I didn’t know that you could actually program cells to do specific things. List of New Cancer Drugs - Health and Life.