

Coding Tibial Plateau Stress Fracture – A Complex Overuse Knee Injury. Diabetic Ketoacidosis– Symptoms, Diagnosis and ICD-10 Codes. Regarded as a life-threatening complication of diabetes, diabetes ketoacidosis (DKA) occurs when your body produces high levels of ketones.
The condition develops when your body does not have enough insulin to process high levels of glucose in the blood. Insulin plays a major role in regulatingthe sugar (glucose - a major source of energy for your muscles and other tissues) - entering your cells. Without adequate insulin, your body begins to break down fat as fuel called ketones, which causes the blood to become acidic. Ketones are normally produced when the body breaks down fat after a long time between meals. Key Podiatry Coding Mistakes You Should Avoid Making - mosoutsource — LiveJournal.
Podiatry medical coding involves the use of the correct patient diagnoses codes, procedure codes and modifiers to get paid for the services provided.
Doctors of podiatric medicine (DPM) may have to go through time-consuming claim submission tasks. Personalized coding, errorless procedures as well as other challenges make podiatry billing a complex one. For better reimbursement for podiatrists, here are some coding mistakes coders should avoid. Podiatry claims should only be submitted with the correct CPT codes that correctly align with the proper ICD-10 codes. If a patient has more than one condition, several diagnosis codes may be required. ICD-10 Codes for Reporting the Top 5 Neurological Disorders.
The term neurological disorder refers to any condition caused by the dysfunction in any part of the brain or nervous system, resulting in physical and/or psychological symptoms.
The brain, spinal cord and nerves together make up the nervous system and control all the workings of the body. When something goes wrong in any part of the nervous system, people may experience trouble moving, speaking, breathing or learning. Medical Codes and Coding Guidelines for CAR-T Therapy. CAR T-cell or Chimeric Antigen Receptor (CAR) T-cell refers to a cell-based gene therapy where a patient’s own T lymphocytes (T-cells) are extracted,genetically modified and infused back into the patient to fight cancer cells.
This treatment is medically reimbursable. Proper code assignment is crucial for any such procedures, as medical coding errors will impact the practice’s revenue and reimbursement. Error-free medical coding services provided by reliable companies will help specialists providing this therapy to meet their medical claim reporting and submission tasks. In August 2019, Medicare announced coverage for CAR-T-Cell Cancer therapy.
How to Document and Code Osteoarthritis, a Degenerative Disease by Outsource Strategies. By Outsource Strategies Medical Billing Company One of the most common chronic joint conditions, osteoarthritis (OA) causes pain, swelling, stiffness and difficulty moving the joint.
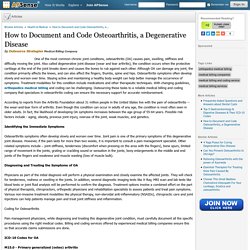
Also called degenerative joint disease (wear and tear arthritis), the condition occurs when the protective cartilage at the end of the joint breaks down and causes the bones to rub against each other. Although OA can damage any joint, the condition primarily affects the knees, and can also affect the fingers, thumbs, spine and hips.
Top 5 Gastroenterology & Digestive Diseases & Their ICD-10 Codes by Outsource Strategies. By Outsource Strategies Medical Billing Company If you are experiencing severe abdominal pain, nausea or bloating, it could be a serious sign of a gastrointestinal condition that may require immediate medical attention.
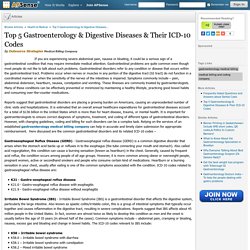
Gastrointestinal problems are quite common even though most people do not like to talk about such problems. ICD-10 Codes to Document Gastritis, a Common Gastroenterology Condition - mosoutsource — LiveJournal. Gastritis is a common condition that occurs due to an inflammation of the protective lining of the stomach.
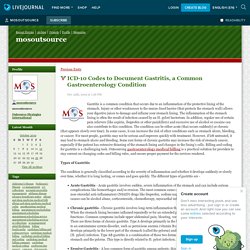
Injury or other weaknesses to the mucus-lined barrier (that protects the stomach wall) allows your digestive juices to damage and inflame your stomach lining. The inflammation of the stomach lining is often the result of infection caused by an H. pylori bacterium. In addition, regular use of certain pain relievers (like aspirin, ibuprofen or other painkillers) and excessive use of alcohol or cocaine can also contribute to this condition. The condition can be either acute (that occurs suddenly) or chronic (that appears slowly over time). Frequently Asked Questions and Answers about Dental Cysts by Outsource Strategies. By Outsource Strategies Medical Billing Company Dental and oral health is an important part of your overall health and well-being.

Normally, the body's natural defenses and good oral health care habits, (such as daily brushing and flossing) can keep bacteria under control. However, poor oral hygiene can cause different oral infections (like tooth decay, gum disease) and has also been linked to other diseases like cancer, diabetes and heart disease. Even minor growths or dental pain can be the sign of a more serious issue in its earliest stages.
Documenting and Coding Peripheral Artery Disease (PAD) - mosoutsource — LiveJournal. Peripheral artery disease (PAD) refers to diseases of the blood vessels (located outside the heart and brain) that occur in the arteries of the circulatory system.
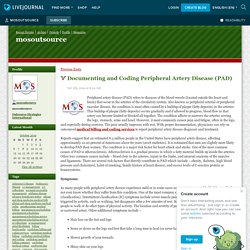
Also known as peripheral arterial or peripheral vascular disease, the condition is most often caused by a buildup of plaque (fatty deposits) in the arteries. This buildup of plaque (fatty deposits) occurs gradually and if allowed to progress, blood flow in that artery can become limited or blocked all together. The condition affects or narrows the arteries serving the legs, stomach, arms and head. However, it most commonly causes pain and fatigue, often in the legs, and especially during exercise. Six Common Dental Problems and Their Related ICD-10 Codes. Dental or oral health is an important part of your overall health and well-being.
Lack of proper oral hygiene can lead to dental cavities, gum diseases and has also been linked to heart disease, cancer, and diabetes. Proper oral hygiene habits (like proper brushing, flossing, limiting the intake of sugar) will help evade costly dental procedures. Patients must be encouraged to go for regular dental check-ups and educating themselves about the common dental problems and their related causes. Dealing with the process of medical billing and coding and insurance coverage is a challenging task for all dental practices. Relying on the services of an established dental billing company can help in accurate clinical documentation and appropriate reimbursement. ICD-10 Codes for Reporting Hodgkin's Lymphoma (Hodgkin's disease) - mosoutsource — LiveJournal. Hodgkin's lymphoma is a type of cancer that develops in the lymphatic system, which is a network of vessels and glands spread throughout your body.
The lymphatic system (which is part of your immune system)is a network of nodes (knots of tissue) connected by vessels that drain fluids and other waste products from the body and fight infections (caused by bacteria, viruses, and fungi). The lymph nodes act as tiny filters, straining out foreign organisms and cells. Clear fluid called “lymph” flows through the lymphatic vessels and contains infection-fighting white blood cells, known as lymphocytes.
The condition is a relatively aggressive type of cancer that quickly spreads throughout the body, if left untreated. Physician Billing Services. A reputable outsourcing company with many years’ experience in the industry, Outsource Strategies International (OSI) offers cost-effective physician billing services that increase efficiency of medical offices. We can efficiently deal with the changing technology, compliance laws and coding requirements of the US healthcare system and follow up on claim delays and denials. Our HIPAA-compliant solutions ensure the security, privacy and confidentiality of the data you provide to us. Call 1-800-670-2809 today and speak to our medical billing representative regarding your requirements. Efficient and Timely Physician At OSI, we perform the following billing functions for your practice and save 30% to 40% of your operational costs.
Coding Accurately for Echocardiography Services - mosoutsource — LiveJournal. Echocardiography (electrocardiogram) or the ECG test is an effective diagnostic tool that uses ultrasound for the initial evaluation of many cardiac signs and symptoms. ECG provides an excellent view of the cardiovascular system. It provides speedy clinically relevant data cost-effectively and with least stress to the patient. Atrial Fibrillation – Types, Symptoms and Medical Codes - mosoutsource — LiveJournal. Atrial fibrillation (AFib or AF) refers to quivering or irregular heartbeat (arrhythmia) that can directly interrupt the normal flow of blood resulting in blood clots, heart failure and other heart-related complications. The condition is characterized by a rapid and irregular heart beat caused when the upper chambers of the heart (the atria) quiver (fibrillate) erratically, at times faster than 200 times per minute.
The heart condition can have a significant impact on a person’s quality of life, causing debilitating pain, heart palpitations, and chronic fatigue, thereby increasing the risk of stroke fivefold. Treatment for this condition includes medications and other interventions that attempt to alter the heart’s electrical system. As physicians focus on treatment, they can rely on an experienced medical billing and coding company to submit the correct ICD-10 diagnosis codes for clinical billing. Types of Atrial fibrillation (AFib) Medical Coding for Laminectomy – A Common Orthopedic Surgical Procedure - mosoutsource — LiveJournal. If you happen to experience mild to severe back pain that generally spreads down to your legs, then it must be a symptom of spinal stenosis. Spinal stenosis is caused by the narrowing of the spaces within the spinal column which puts pressure on the spinal cord or nerves. The condition generally occurs due to the wear and tear changes in the spine and other causes including herniated disks, thickened ligaments, overgrowth of bone, tumors and spinal injuries.
This spinal disorder is most common in men and women above 50 years of age. ICD-10 Codes for Four Common Orthopedic Problems of the Elderly - mosoutsource — LiveJournal. Documenting and Coding Orbital Fracture – A Common Eye Condition - mosoutsource — LiveJournal. Documenting Gastrointestinal Stromal Tumor (GIST) with ICD-10 Codes - mosoutsource — LiveJournal. Polyhydramnios – What You Need to Know - mosoutsource — LiveJournal. Medical Codes for Reporting and Coding Inguinal Hernia - mosoutsource — LiveJournal. Diagnosing, Documenting, and Coding Sciatica. Reporting Chondromalacia Patella with ICD-10 Codes. Documenting Cataracts with ICD-10 and CPT Codes. WHO Recognizes Workplace Burnout as an “Occupational Phenomenon” Documenting and Coding Bradycardia – Use These Medical Codes. Reporting Pancreatic Cancer – Use the Correct ICD-10 Codes. Medical Codes for Gallstones – A Common Condition of the Gallbladder. ICD-10-PCS Coding Guidelines for Coronary Arterial Bypass Procedures.
How to Code Temporomandibular Joint Disorders Using ICD-10 Codes. How to Correctly Code Bunions - A Common Bone Deformity by Outsource Strategies International. How to Correctly Code Bunions - A Common Bone Deformity. Medical Codes to Document Esophageal Cancer – An Overview. Billing Codes for Neurofibromatosis – A Genetic Neurological Condition. Documenting Acute Kidney Injury with Accurate Medical Codes. Documenting and Billing for Facet Joint Injections. ICD-10 Codes for Documenting Hypoglycemia Caused by Low Blood Sugar. Psychiatry Medical Billing and Coding - Key Services to Document. Documenting Myasthenia gravis (MG) with ICD-10 Codes. Get to Know Those ICD-10 Codes to Report Crohn's Disease. Documenting Meniscectomy Procedure – Know the Medical Codes. Medical Coding for Ambulatory Phlebectomy Procedure. Documenting Kyphosis – An Overview of Treatment and Coding. Know the ICD-10 Codes to Document and Code Ovarian Cysts.
Frequently Asked Questions and Answers about Esophagectomy. Reporting Diabetic Ketoacidosis (DKA) with the Correct ICD-10 Codes. Learn the ICD-10 Codes to Code Gestational Diabetes Mellitus (GDM) Documenting and Coding Amyloidosis - Use the Correct ICD-10 Codes. Documenting Osteomyelitis - Symptoms, Diagnosis and ICD-10 Codes. Medical Coding for Gastroenteritis - Know More about the ICD-10 Codes. Documenting and Coding Ankylosing Spondylitis (AS) Pulmonary Valve Stenosis - Learn About the ICD-10 and CPT Codes. Documenting and Coding Bronchoscopy Procedures. Coding Malignant Hyperthermia for Optimal Reimbursement.
Cleft Lip and Cleft Palate Repair – Diagnosis and Medical Coding. Documenting Parkinson’s Disease (PD) with the Correct ICD-10 Codes. How to Code Coronary Artery Disease Using ICD-10 and CPT Codes. How to Code Lyme Disease Using the Correct Medical Codes. How to Document Diverticulitis with Accurate ICD-10 Codes. How to Document Cholecystitis Using ICD-10 and CPT Medical Codes. An Overview of ICD-10 Codes for Diagnosing and Documenting Hernia. Documenting and Coding of Bipolar Disorder Using ICD-10 Codes. Debridement - Proper Documentation Crucial for Accurate Coding. Learn How to Diagnose and Document Sleep Apnea Using the Correct ICD-10 Codes. Documenting Mental and Behavioral Health Issues with ICD-10 Codes. How to Bill and Code for Pap Smears. Documenting Cushing’s Syndrome with ICD-10 Codes – an Overview.
What Is Dystonia and How to Report It with the Correct ICD-10 Codes. An Overview of Spinal Stenosis and How to Report It Using ICD- 10 Codes. Documenting Ulcerative Colitis Using ICD-10 Codes – An Overview. Type 2 Diabetes – Causes, Diagnosis and ICD-10 Documentation. Sarcoidosis Diagnosis and Coding – An Overview of ICD-10 Codes.
New CPT® Codes and Descriptors for 2018 Released by AMA. Documenting and Coding Asthma in ICD-10. Advance Care Planning (ACP) – Frequently Asked Questions & Answers. Medical Coding for Irritable Bowel Syndrome (IBS) How to Document Gastrointestinal Carcinoid Tumors Using ICD-10 Codes. Diagnosis and Medical Coding for High Risk Pregnancy. General Coding Guidelines for Osteoporosis – An Overview. How to Improve Healthcare Revenue Cycle Management. Routine Screening Crucial for Early Detection of Prostate Cancer. How to Document Parkinson’s Disease using ICD-10 Codes. Strategies to Improve Medical Billing, Payment and Patient Satisfaction.
How to Document Christmas Injuries with ICD-10. ICD-10 Coding Guidelines for Alzheimer’s Disease. Coding for Chronic Obstructive Pulmonary Diseases – An Overview. New Medicare Fraud Audit Update Could Reduce Burden on Compliant Providers. Chiropractic Billing Coverage Guidelines by Private Insurers. Study Finds Chiropractic Care a Safe and Effective Option for Pain Relief.
Financial Incentives Boost the Rate of Colorectal Cancer Screenings. Learn More about Enterocolitis and its ICD-10 Documentation. Documenting Melanoma This UV Safety Month. A Review of EHR Medical Coding and Its Challenges. Modifier 25 – Understand the Facts to Avoid Misuse. CMS’ Proposed Rules on Quality Payment Program for 2018. Prior Authorization – Are Physicians Frustrated with the Process? Eye Stroke – Causes, Treatment, Documentation and Coding. Screening Mammography Medicare Coverage and Documentation Guidelines - mosoutsource. Dental Office Accounts Receivable (AR) and the Role of a Front Office Manager. Prevalence of HDV Infection in the U.S. – An ICD-10 Analysis.