

MPR 23.03.21 Case Report Pain Med Dose Linked to Patient's Sleepwalking. SAS Dolor Autoaudit Iniciotratamientoopioides 01012021. J.jacc.2020 Complicaciones CV de opioides. MPR FDA Strengthens REMS for Transmucosal Immediate Release Fentanyl Products. MPR 23 07 20 Do Opioids Have a Role in the Management of Knee and Hip Osteoarthritis. 2020 BMJ Open uso concurrente de BZP, Z, opioides. Opioides: ¿cómo hacer un seguimiento adecuado? 14.10,20 MPR FDA Rejects IV Tramadol Over Potential Safety Concern MPR. Transdermal fentanyl patches for non-cancer pain: do not use in opioid-naive patients. Advice for healthcare professionals: Review of opioid medicines Considerable concern has been raised regarding the prescribing of opioids in the UK (see Drug Safety Update on risk of dependence and addiction with opioids).
In 2019, the Commission on Human Medicines (CHM) convened an Expert Working Group to examine the benefits and risks of opioids in the relief of non-cancer pain. During this review it was noted that there have been reports of serious harm, including fatalities, associated with fentanyl patches in both opioid-naive patients and opioid-experienced patients.
Up to May 2020, we have received 13 Yellow Card reports in which opioid-naive patients have experienced respiratory depression following use of fentanyl and additional Yellow Card reports in which respiratory depression was reported in patients switched from another opioid to an inappropriately high dose of fentanyl. The initial dose of fentanyl should be based on a patient’s opioid history. Am Fam Phys 2020 Dolor crónico y opioides. Arthritis Care Res 2020 Opioides en artrosis. MPR 28.04 Opioides vs AINEs ERC observacional. AHRQ Patient Safety Opioids abril 2020opioids. AHRQ opioids chronic pain Abril 2020. MTRAC Tapentadol guidance Jan 2019. 5 steps to tapering opioids for patients with chronic non-cancer pain - NPS MedicineWise. Read an accessible text version of this algorithm Tapering rates Fast taper If tapering is required after a shorter period of opioid treatment ie, less than 3 months, or if treatment goals of an opioid trial have not been achieved, then a faster rate of tapering is recommended,7 that is, reducing the daily opioid dose each week by 10%–25% of the dose you are starting the taper from.
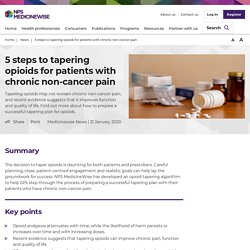
However, if tapering is required in response to significant adverse effects, daily stepwise reduction may be more appropriate.7 Slow taper In situations where longer term opioid treatment has been maintained (often for many years) without meaningful improvement in pain and function, the recommended approach is slow tapering and stopping completely if possible. One practical strategy is to reduce the daily opioid dose each month by 10%–25% of the dose you are starting the taper from. Consider specialist advice when changing opioid treatment. Monitor regularly Establish success criteria Tapering takes time and patience. Wei J Tramadol y riesgo de Fx JBMR. Tapering opioids Am Fam Phys ene 2020. Tramadol fibromialgia. OSU opioides DCNO. Manejo estreñimiento por opioides JAMA 2019. Fleischman 2019 oi 190072. Boletín CSS cuatrimetral nº 9 1 2019. Tramadol opioid lite BMJ 2019. Frost Tramadol interactions Pharmacotherapy2019.
Tapentadol CDEC Final Recommendation October 25, 2018. BOLCAN OPIOIDES INTERAIVO Y PPT 2016. Ojo Markov 9 pasos para el éxito en la prescripción de opioides en DCNO. FDA Opioids 2016. 2017 RxFiles Pain Management & Opioids. Opioids. Tramadol. JAMA 2018 opioides vs no opioides. Opioids DSC clean. 2017 07 30 Opioides y benzodiazepinas Rhode Island. CDC Guideline for Prescribing Opioids for Chronic Pain — United States, 2016. The recommendations are grouped into three areas for consideration: Determining when to initiate or continue opioids for chronic pain.Opioid selection, dosage, duration, follow-up, and discontinuation.Assessing risk and addressing harms of opioid use.

There are 12 recommendations ( Box 1). Each recommendation is followed by a rationale for the recommendation, with considerations for implementation noted. In accordance with the ACIP GRADE process, CDC based the recommendations on consideration of the clinical evidence, contextual evidence (including benefits and harms, values and preferences, resource allocation), and expert opinion. For each recommendation statement, CDC notes the recommendation category (A or B) and the type of the evidence (1, 2, 3, or 4) supporting the statement ( Box 2). In summary, the categorization of recommendations was based on the following assessment: Determining When to Initiate or Continue Opioids for Chronic Pain 1. 2. 3. 4. 5. 6. 7. 8. Pregnant Women 9. 10. Guidelines Factsheet a. Opioid GL for CMAJ 01may2017. Tramadol wemerec 2013. OSU 2017 03 23 Tramadol Evaluation. OSU opioides en DCNO 2017. OSU 2016 05 26 Opioides 2015 ClassUpdate. San José FMC 12.17 opioides.
Opioides mayores disponibles 2017.jpg large. Tramadol CMAJ 2013. PRACTICAS SEGURAS OPIOIDES dolor crónico. Opioides en DCNO. FMC 12 2016. FDA opioides y bdz 2016. FDA Drug Safety risks opioid with benzodiazepines 2016. FDA adicción opioides y bdz 2017. CADIME BTA2011 27 4. CADIME BTA 2015 30 4 (1)