

When To Introduce a Bottle To a Breastfed Baby? A few months ago I received a call from a confused mum; her baby was 3 months old, breastfed, and that night he had refused his daily bottle.
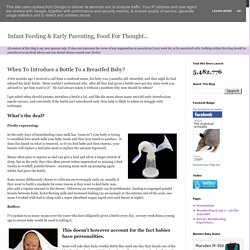
Mum couldn't understand why, after all they had given a bottle once per day since week 2 as advised to "get him used to it". He had always taken it without a problem why now should he refuse? I get asked when should parents introduce a bottle a lot, and like the mum above many are told early introduction equals success, and conversely if the bottle isn't introduced early then baby is likely to refuse or struggle with technique. What's the deal? Firstly expressing: In the early days of breastfeeding (once milk has "come in") your body is trying to establish how much milk your baby needs and thus how much to produce. Some mums deliberately choose to cultivate an oversupply early on, usually if they want to build a stockpile for some reason ie they want to feed baby now, plus add a regular amount to the freezer.
Nipple confusion, real or not? Tools for Feeding: Bottles & More. Finger feeding (Photo used with permission) Following are some resources for alternative feeding methods, including bottle feeding, cup/dropper/spoon feeding, finger feeding, supplementing at the breast, and ideas for older babies.
Bottle | Cup, Dropper, Spoon | Finger Feeding | At Breast | Back to Breast | Older Babies Bottle feeding How to bottle-feed the breastfed baby Alternatives to bottles for younger babies (including preemies) Cup, dropper, syringe, and links with various methods Alternatives to bottle from AskDrSears.comRefusing a Bottle: Dropper & Cup Feeding by Paula YountFinger and Cup Feeding by Jack Newman, MD, FRCPCCup Feeding from the Breastfeeding Committee for SaskatchewanCup Feeding Instructions and FAQs from foleycup.com Comparison of the Safety of Cup and Bottle Feedings in Premature Infants Whose Mothers Intend to Breastfeed information on study by Kathleen A.
SNS. Alternative feeding methods. How much expressed milk will my baby need? By Kelly Bonyata, BS, IBCLC Image credit: Jerry Bunkers on flickr How much milk do babies need?
Many mothers wonder how much expressed breastmilk they need to have available if they are away from baby. In exclusively breastfed babies, milk intake increases quickly during the first few weeks of life, then stays about the same between one and six months (though it likely increases short term during growth spurts). Current breastfeeding research does not indicate that breastmilk intake changes with baby’s age or weight between one and six months. The research tells us that exclusively breastfed babies take in an average of 25 oz (750 mL) per day between the ages of 1 month and 6 months. We can use this information to estimate the average amount of milk baby will need at a feeding: Example: If baby usually nurses around 8 times per day, you can guess that baby might need around 3 ounces per feeding when mom is away. (25/8=3.1). What if baby is eating solid foods? Fast flow bottles. Be patient. Milkstorage01. Reusing expressed breastmilk.
Q: Should breastmilk left over from a feeding be dumped immediately (like formula), or can you save it and give it to baby later?
A: It is probably safe to save the left-over milk for use at the next feeding, but no published studies have investigated this issue. Storage of left-over milk is a different issue than storage of fresh milk because bacteria from baby’s mouth usually enters the milk once baby begins drinking. Freshly expressed milk contains live cells which kill bacteria, and one study (Pardou et al, 1994) found that some of the milk that had been refrigerated for 8 days actually had lower bacteria levels than when the milk was first expressed.
Many mothers of healthy babies have saved left-over milk for longer than two hours (sometimes as long as 24-48 hours) with no problems, but whether or not the milk is safe depends on several factors. Fresh breastmilk has the most bacteria-fighting power, followed by refrigerated milk, then previously-frozen milk. Brusseau R. The Breastfeeding Mother: The Trouble with Calma and the Quest for the Perfect Bottle Nipple. When breastfeeding moms either want or need for their baby to have expressed milk from a bottle, the question they usually ask is, “What bottle/nipple is most like the breast?

Which bottle/nipple is best for breastfeeding babies?” The simple truth is that the correct answer is, “None.” There is no nipple that is like the human breast. Some may be better or worse for a baby who is going back and forth between breast and bottle, but there is no “best. " Getting baby to take a bottle.