

What Does Chemotherapy Feel Like? « Chronicles of a Cancer Patient. What Does Chemo Do To You?
Ok, this one might be a little too much information for you. But if there’s somebody out there that will be going through all this, you should read this. Or maybe you shouldn’t. People ask me on the bad days what chemotherapy is like, and although I consider myself articulate, I have a really difficult time explaining it. Its difficult to describe the forest from the trees, right? Chemotherapy side effects are worse than cancer, that’s for sure. Chemo, on the other hand, you can never forget that. Well, I’ll tell you what I can about chemo. I’ll start on Sunday, the day before chemo.
The dread of chemotherapy now starts much earlier than Sunday. And I suppose I should feel good that I only have 2 more treatments. I try to distract myself on Sundays, and thankfully, I think everyone around me tries to do the same. I sleep as late as I can on Mondays. Chemotherapy is about a 4 hour process. The heat starts about then. I don’t really know when it happens. Epidemiology, risk factors and the clinical approach to ER/PR negative, HER2-negative (Triple-negative) breast cancer. Triple-negative breast cancer is defined by absent expression of the estrogen receptor (ER), progesterone receptor (PR), and human epidermal growth factor receptor 2 (HER2).

These cancers tend to behave more aggressively than other types of breast cancer. Unlike other breast cancer subtypes (ie, ER-positive, HER2-positive subtypes), there are no targeted treatments available, other than the administration of chemotherapy. Although the basic principles of diagnosis and management of triple-negative breast cancer are similar to those of breast cancer in general, many aspects, including risk factors, molecular and pathologic characteristics, natural history, and chemotherapy sensitivity, are unique to triple-negative breast cancer and will be reviewed here.
A more extensive discussion on surgical management, neoadjuvant chemotherapy, adjuvant chemotherapy of the non-metastatic breast cancer, and the treatment of metastatic breast cancer is covered separately. Update on triple-negative breast cancer: prognosis and management strategies. Implant-based breast reconstruction following radiation has high patient satisfaction rate despite complications. Breast cancer patients who have received radiation therapy after mastectomy have more problems related to the use of implants for breast reconstruction, according to a review in the October issue of Plastic and Reconstructive Surgery®, the official medical journal of the American Society of Plastic Surgeons (ASPS).

Although women should be aware of these increased risks, implant-based breast reconstruction after radiation therapy is still successful in most cases, according to the paper by Dr. Steven J. Kronowitz of The University of Texas MD Anderson Cancer Center, Houston. Incidence and Consequence of Close Margins in Patients with Ductal Carcinoma-In Situ Treated with Mastectomy: Is Further Therapy Warranted? Outcomes in Patients Treated With Mastectomy for Ductal Carcinoma In Situ - International Journal of Radiation Oncology. To view the full text, please login as a subscribed user or purchase a subscription.

Click here to view the full text on ScienceDirect. Fig. 1 Effect of age ≤40 years on 10-year locoregional recurrence. Purpose To examine, in a large, population-based cohort of women, the risk factors for recurrence after mastectomy for pure ductal carcinoma in situ (DCIS) and to identify which patients may benefit from postmastectomy radiation therapy. Methods and Materials Data were analyzed for 637 subjects with pure DCIS, diagnosed between January 1990 and December 1999, treated initially with mastectomy. Results Median follow-up was 12.0 years. Conclusion Mastectomy provides excellent locoregional control for DCIS. Purchase access to this article You must be logged in to purchase this article. Claim Access If you are a current subscriber with Society Membership or an Account Number, claim your access now. Subscribe to this title Institutional Access. Recurrence after Mastectomy for Ductal Carcinoma <i>In Situ</i>: ingentaconnect.
GetSharedSiteSession?rc=4&redirect=http%3A%2F%2Fwww.redjournal. To view the full text, please login as a subscribed user or purchase a subscription.

Click here to view the full text on ScienceDirect. Hypofractionated whole-breast irradiation (HF-WBI) offers an opportunity for improved patient convenience, lower healthcare costs, and greater access to care without sacrificing outcomes. This approach typically involves 40 to 43 Gy delivered at 2.5 to 2.7 Gy per fraction over 3 weeks. Is Ductal Carcinoma In Situ (DCIS) Breast Cancer? (March 2013) What is ductal carcinoma in situ (DCIS)?
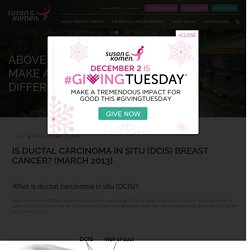
Image source: National Cancer Institute ( DCIS in the United States It is estimated that there will be about 55,000 new cases of DCIS diagnosed among women in the U.S. in 2013.1. Radiation Oncology/Breast/DCIS - Wikibooks, open books for an open world. Understanding DCIS. Generally, lumpectomy is the first step in breast-conservation therapy.

Lumpectomy is usually performed in an outpatient setting using local anesthesia. However, general anesthesia can be used for greater patient comfort. If cancer cells are present at the margin (the edge of the biopsied tissue), a re-excision needs to be done to remove the remaining cancer. If you are large-breasted, most of your breast can be preserved and you will still have the image you are accustomed to. If you are small-breasted and need additional surgery, lumpectomy may not result in a good cosmetic result; mastectomy with reconstruction can be a good option.
Is radiation indicated in patients with ductal carcinoma in situ and close or positive mastectomy margins? Compass: Ductal Carcinoma In Situ. Ductal Carcinoma In Situ Choosing Treatment for a Common Group of Early, Confined Breast Cancers Overview By definition, ductal carcinoma in situ (DCIS) is a cancer arising from and pathologically confirmed to be confined to the terminal duct lobular units of the breast.
It is therefore considered a noninvasive breast cancer. Each year in the United States, about 64,000 women are diagnosed with DCIS, representing 30% of women diagnosed with breast cancer. Three decades ago, DCIS was found in patients relatively rarely, typically co-existing with invasive cancers in mastectomy specimens. Today, it is still unusual for DCIS to present symptomatically; approximately 90% of these cancers are discovered as microcalcifications on mammograms. Long-term outcome after postmastectomy radiation therapy for the tr... Is radiation indicated in patients with ductal carcinoma in situ an... Breast brachytherapy with strut-based applicator effective for women with DCIS. Breast brachytherapy with a strut-based applicator appears to be an effective treatment for women who have ductal carcinoma in situ (DCIS) of the breast, according to a groundbreaking study presented at the annual meeting of the American Society of Breast Surgeons, held in Phoenix May 2-4.
The study is the largest ever presented on the use of breast brachytherapy to treat DCIS. The impact of immediate breast reconstruction on the technical delivery of postmastectomy radiotherapy - International Journal of Radiation Oncology. To view the full text, please login as a subscribed user or purchase a subscription.

Click here to view the full text on ScienceDirect. Fig. 1 (a) An “optimal” treatment plan received no point deductions in chest wall coverage, treatment of the ipsilateral internal mammary chain (IMC), minimization of lung volume, and avoidance of epicardial structures. (b) A treatment plan with “major” compromises received 2.5 point deductions. A full point was deducted for irradiating more than 1 cm of heart. Impact of Margin Status on Local Recurrence After Mastectomy for Ductal Carcinoma In Situ - International Journal of Radiation Oncology. To view the full text, please login as a subscribed user or purchase a subscription. Click here to view the full text on ScienceDirect. Purpose. Close or Positive Margins After Mastectomy for DCIS: Pattern of Relapse and Potential Indications for Radiotherapy - International Journal of Radiation Oncology. Close or Positive Margins After Mastectomy for DCIS: Pattern of Relapse and Potential Indications for Radiotherapy - International Journal of Radiation Oncology.
Postmastectomy Radiation Therapy: An Overview for the Practicing Surgeon. Impact of margin status on local recurrence after mastectomy for du...